Some side effects announce themselves loudly. Others sneak in wearing a “normal day” mask. You wake up tired, but you’re in Cancer treatment, so of course you’re tired. Your heart races, but you’re anxious, so that fits, right?
Still, there’s a moment when your body feels like it’s running on the wrong setting, like a thermostat that can’t decide between heat and cold. Immunotherapy thyroiditis, an immune-related adverse event, can cause that kind of whiplash, and it’s easy to miss at first.
This guide connects the dots between sudden fatigue, a fast heartbeat, and weight changes. It also lays out the thyroid labs worth requesting, so you can walk into your next visit with steadier footing.
Why immunotherapy thyroiditis can feel like your body has two gears
Immunotherapy drugs like immune checkpoint inhibitors push your immune system to recognize and attack cancer cells. Examples include PD-1 inhibitors such as nivolumab and pembrolizumab, anti-PD-L1 monoclonal antibodies, and anti-CTLA-4 therapy like ipilimumab. That same immune “wake up” can also irritate healthy tissues. For some people, the thyroid becomes the unintended target.
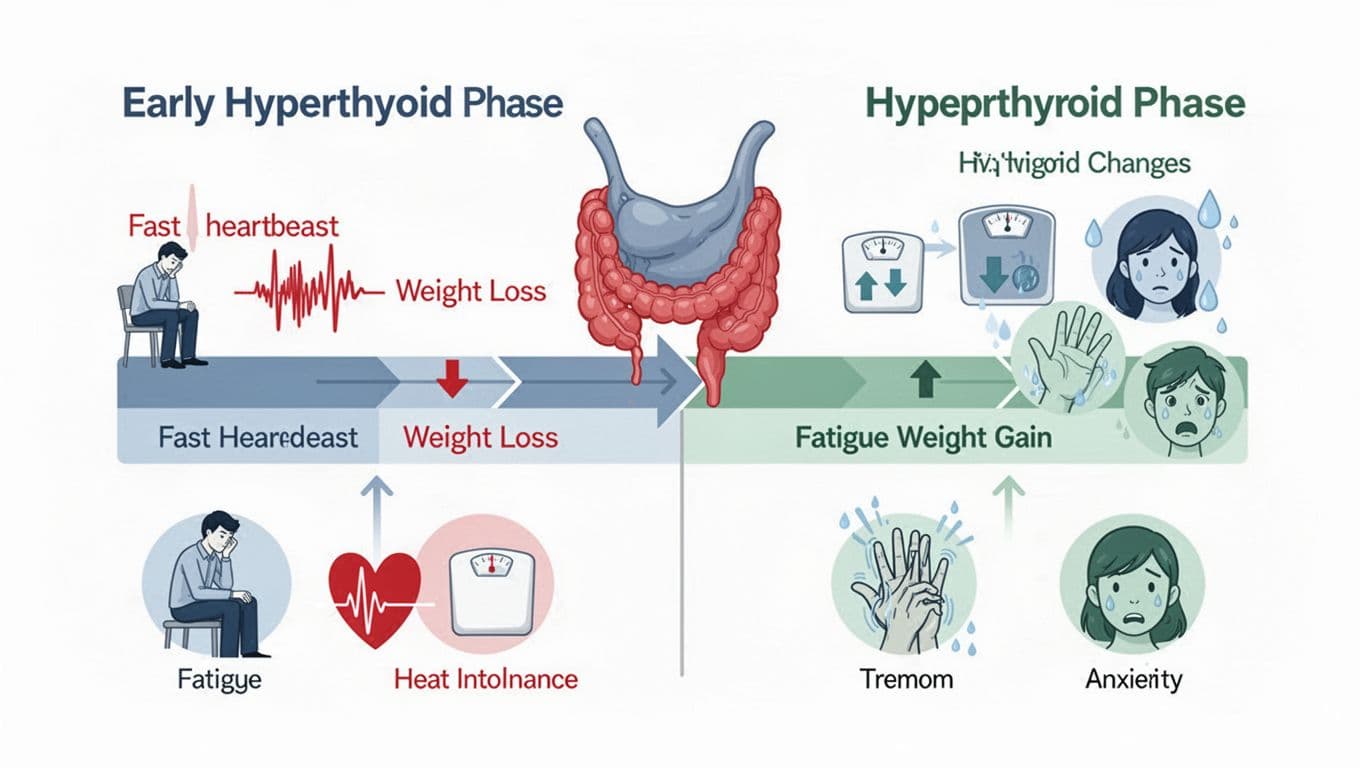
When that happens, the story often unfolds in two chapters.
First, there may be a hyperthyroid phase, often a form of thyrotoxicosis caused by painless thyroiditis or destructive thyroiditis (too much thyroid hormone in the blood). This can feel like hyperthyroidism, with your body revving high even when you’re sitting still. You might notice a fast heartbeat, shaky hands, more sweating, heat intolerance, trouble sleeping, or weight loss even if you’re eating normally. Some people also feel keyed up, restless, or edgy in a way that doesn’t match their day.
Then, the thyroid can swing the other direction into a hypothyroid phase (too little thyroid hormone). That’s when fatigue can flatten you. Weight gain can show up quickly. Constipation, dry skin, cold intolerance, low mood, or brain fog may follow. Even your voice can feel a bit rougher, like your body is speaking through cotton. This phase may settle into hypothyroidism.
Not everyone gets both phases. Timing also varies. Symptoms can begin weeks after starting immunotherapy, or later, and they can show up even when you’re feeling hopeful, even during remission, when you want your body to “just behave.”
For a deeper medical overview of how this happens, see the 2025 review on immune checkpoint inhibitor induced thyroiditis mechanisms. You can also read the open access summary in an updated review of immunotherapy induced thyroid dysfunction.
If your heart is racing and your legs feel heavy, it’s not weakness. It’s your body waving a flag that deserves attention.
The thyroid labs to ask for, plus what each one helps answer
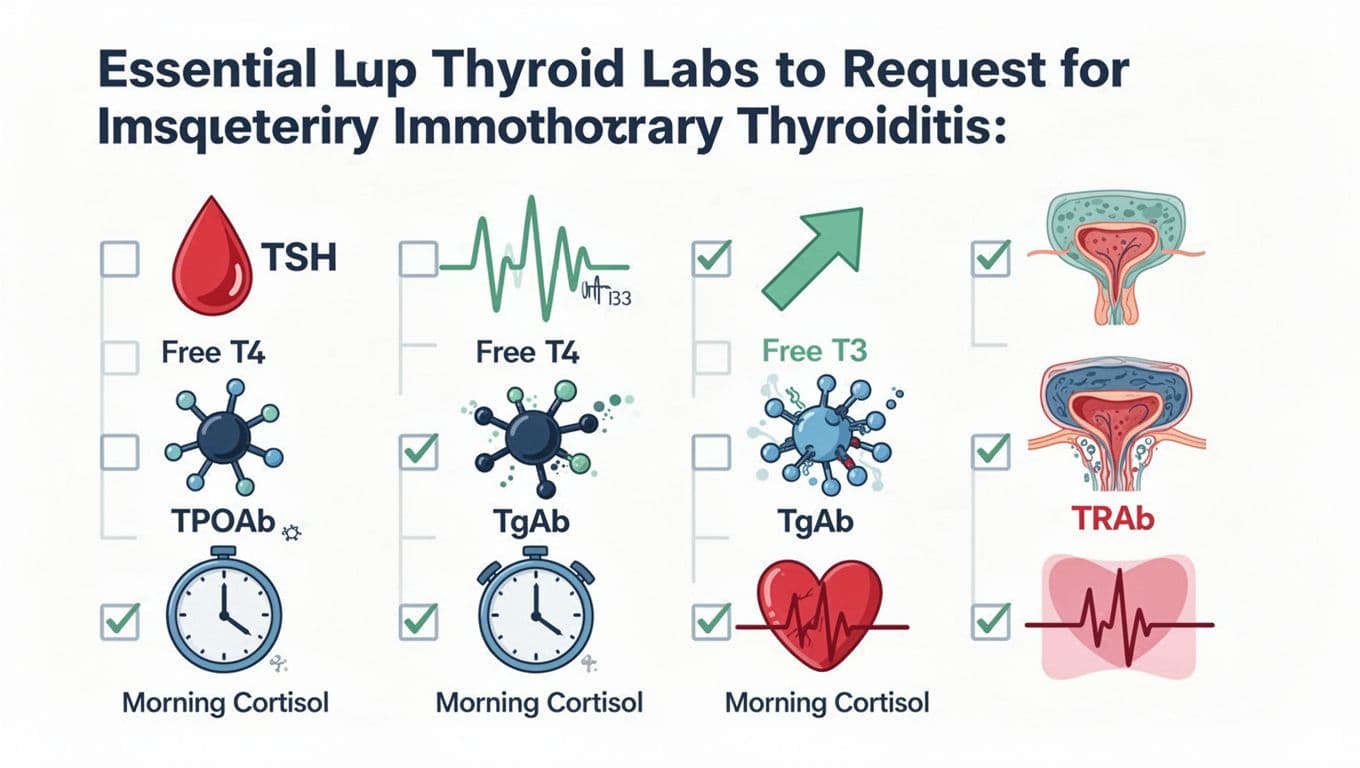
When symptoms hit, many people ask for “thyroid function tests” and get only one number back. That’s a start, but it’s often not enough when immunotherapy is involved.
A simple, clear request to your oncology team sounds like: “Could we check thyroid stimulating hormone, free thyroxine, and T3, and add thyroid antibodies? I’m having palpitations, fatigue, and weight changes.”
Here’s what those thyroid function tests can help clarify.
| Test to request | What it helps show | Why it matters in immunotherapy thyroiditis |
|---|---|---|
| thyroid stimulating hormone (TSH) | Your pituitary’s signal to the thyroid | Often shifts early, but it can lag behind symptoms |
| free thyroxine (Free T4) | Usable thyroxine level | Helps confirm hyper or hypo states |
| Total or Free T3 | Triiodothyronine level | Useful when symptoms suggest hyperthyroid phase |
| antithyroid peroxidase antibodies (TPOAb) | Autoimmune thyroid tendency | Can support the diagnosis, but may be negative |
| thyroglobulin antibodies (TgAb) | Another autoimmune marker | Adds context, especially with mixed patterns |
| TRAb or TSI | Graves type antibodies | Helps separate thyroiditis from Graves disease |
| Morning cortisol and ACTH (optional) | Adrenal function | Important because adrenal issues can mimic fatigue and weakness |
| ECG (test, not a lab) | Heart rhythm | Useful if palpitations feel intense or irregular |
While thyroid function tests are primary, a thyroid ultrasound or checking a previous PET/CT scan can provide additional structural context.
The takeaway: ask for a small panel, not a single test. Patterns matter more than any one number.
Also, symptoms don’t always match the lab timing perfectly. If your first set looks “borderline,” perhaps indicating subclinical thyroid dysfunction, your team may repeat labs soon, because thyroiditis can change fast.
If you want a clinician-focused reference you can bring to an appointment, the Immune Checkpoint Inhibitor Toxicity Management guideline (PDF) includes endocrine side effect pathways and monitoring ideas.
When to seek urgent care, and what treatment often looks like

Some thyroid symptoms are miserable but manageable. Others need faster action, especially when a racing heart enters the room.
Seek urgent care right away if you have chest pain, fainting, severe shortness of breath, confusion, a pounding heartbeat that doesn’t settle, or symptoms of thyroid storm as a rare but serious complication. A high fever with severe weakness also deserves urgent evaluation. Those signs can point to problems beyond the thyroid, and immunotherapy patients should never “tough it out” alone.
When it is immunotherapy thyroiditis, an immune-related adverse event common in patients with metastatic melanoma, non-small cell lung cancer, or renal cell carcinoma treated with PD-1 inhibitors such as nivolumab and pembrolizumab, or anti-CTLA-4 therapy like ipilimumab, treatment depends on which phase you’re in.
During the hyperthyroid phase, many people don’t need anti-thyroid drugs because the issue is often hormone “leak” from inflammation, not overproduction. Interestingly, studies have linked developing hyperthyroidism or thyrotoxicosis during such treatments, including nivolumab for metastatic melanoma and non-small cell lung cancer, to improved overall survival and progression-free survival. Instead, clinicians often focus on symptom relief, for example using a beta-blocker to calm palpitations and tremor. Your team may also look for dehydration, infection, anemia, or heart rhythm changes, because those can stack on top of thyroid shifts.
Later, if the thyroid slows down with hypothyroidism, levothyroxine replacement therapy can help bring back energy, bowel regularity, temperature comfort, and mental clarity for hypothyroidism management. Hypothyroidism is frequently managed this way, and dosing is personal; it may change as your body settles from hypothyroidism after immunotherapy, another common immune-related adverse event.
One more brave but practical note: fatigue can come from more than one place at once. That’s why the optional cortisol and ACTH tests matter. Low cortisol can look like “I can’t get off the couch,” and it needs a different fix than thyroid hormone.
For a broader discussion of hypothyroidism after immunotherapy and common management approaches, see immunotherapy related hypothyroidism mechanisms and management.
Conclusion
A fast heartbeat signaling hyperthyroidism, sudden fatigue, and weight changes indicative of hypothyroidism can feel like betrayal when you are already carrying so much from immune-related adverse events like those seen with nivolumab or pembrolizumab. Still, naming the pattern, identifying hypothyroidism or hyperthyroidism, is an act of courage, not worry. Ask for the thyroid labs that tell the full story, then ask again if symptoms of hypothyroidism change. Managing these immune-related adverse events requires a multidisciplinary approach involving both oncology and endocrinology. With the right testing and support for hypothyroidism, many people stabilize and keep moving forward, whether they are in treatment or building life in remission.

