If you’re on immunotherapy, you’ve already made a brave choice. You’re trusting your immune system to fight cancer harder than it ever has. Still, even good fighters can misfire.
That’s where immunotherapy nephritis comes in. Choosing immunotherapy involves risk; it harnesses immune checkpoint inhibitors to fight cancer aggressively, but these drugs can misfire and cause acute kidney injury through kidney inflammation. It can start quietly. You might feel “off” before any pain shows up. Sometimes the first clue is a lab number that drifts the wrong way.
This guide walks through the early signs to watch for, plus the kidney labs worth asking about, so you can act early and protect your treatment plan.
Immunotherapy nephritis, the quiet kidney side effect
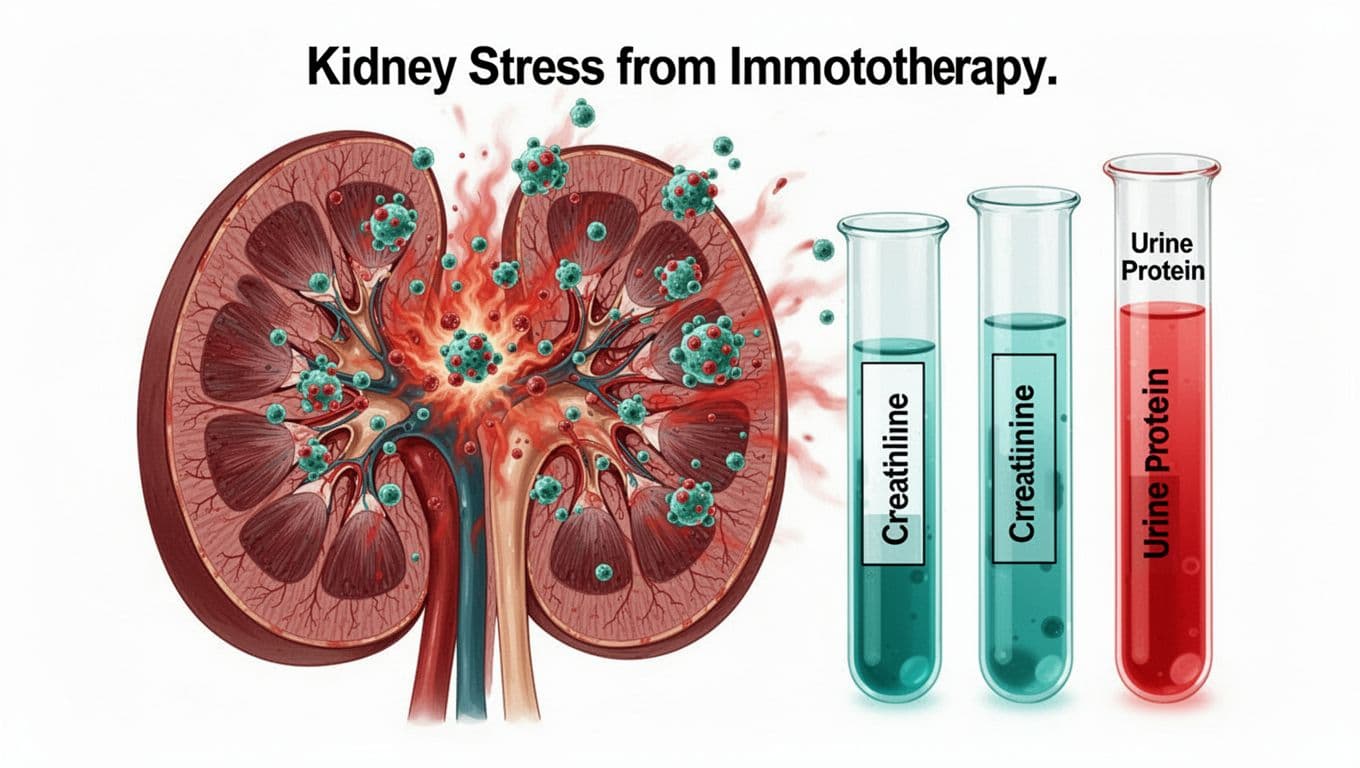
Think of your kidneys like two steady coffee filters. All day, they clean your blood, balance salts, and manage fluid. They do it so quietly that most of us never think about them, until something changes.
With immune checkpoint inhibitors, your immune system becomes more alert. That’s the point. However, in a small number of people, immune cells also irritate healthy tissue. In the kidneys, that irritation can cause interstitial nephritis (formally known as acute tubulointerstitial nephritis) and a sudden drop in renal function.
The tricky part is timing. This nephrotoxicity can show up weeks or months after starting treatment, even in patients with high PD-L1 expression or those being treated for melanoma, and sometimes after a dose change or a new medication is added. Symptoms may be mild at first, so routine labs often catch it before your body does.
Most clinicians watch serum creatinine closely because it rises when the kidneys struggle. Even a “small” jump matters if it’s a clear change from your usual level. If you want a deeper medical summary of how checkpoint inhibitors can affect the kidneys, see this StatPearls overview of ICI kidney injury.
Here’s the heart of it: interstitial nephritis is often treatable, especially when caught early. The courage is in noticing, asking, and not waiting.
A rising creatinine trend is like smoke in the kitchen. You don’t need flames to take it seriously.
Immunotherapy nephritis signs you can spot early

Some side effects announce themselves. Others whisper. Kidney inflammation, a potential acute kidney injury, often whispers.
You might notice these immune-related adverse events as fatigue that feels different from normal treatment tiredness. Maybe it lands heavier, or doesn’t lift with rest. Appetite can fade, and nausea can creep in without a clear reason. On some days, food just feels like too much work.
Fluid changes can be another clue. Swelling in feet or ankles can show up as tighter shoes or sock marks that linger. Weight may rise fast over a few days because your body holds onto water. Meanwhile, urine can change in volume, even if you’re drinking about the same.
Blood pressure is easy to overlook, yet it matters. If your readings climb, or headaches start along with higher numbers, tell your team. Kidneys help regulate blood pressure, so kidney stress can push it up.
A few signs are especially worth mentioning promptly:
- Less urine than usual: A noticeable drop, especially over a day or two. Watch for hematuria or foamy urine indicating proteinuria.
- New swelling: Ankles, legs, hands, or puffy eyelids.
- Shortness of breath: Sometimes tied to fluid buildup.
- Fever: New or persistent without obvious cause.
- Rash: Skin changes, particularly if widespread or itchy.
- Nausea or poor appetite: When it’s new, persistent, or paired with lab changes.
- Higher blood pressure: Especially if it’s new for you.
These signs don’t prove nephritis. Infection, dehydration, diarrhea, and other meds can also strain the kidneys. Still, your job isn’t to diagnose it. Your job is to raise your hand early.
Kidney labs to ask for, and the red flags that need a call
If nephritis is the “why,” labs are the “proof.” The goal is simple: get a baseline, watch trends, and respond fast if numbers shift.
Ask your oncology team which kidney labs they’re following, and request a copy of results. You deserve to see the pattern, not just hear “it looks fine.”
Here are the key labs and what they tell you:
| Lab to ask for | What it helps show | Why it matters in immunotherapy nephritis |
|---|---|---|
| Serum creatinine | Kidney filtering function | Often rises first, even when you feel okay |
| eGFR | Estimated kidney function | Useful for trend, but it’s calculated, not a direct measure |
| BUN | Waste buildup, hydration clues | Can rise with kidney stress or dehydration |
| Potassium and sodium | Salt balance | Dangerous shifts can happen with kidney injury |
| Bicarbonate (CO2) | Acid balance | Low levels can signal kidney-related acid problems |
| Urinalysis (protein, blood) | Early kidney irritation | Protein or blood can support concern for nephritis |
| Urine protein-to-creatinine ratio (UPCR) | Amount of protein loss (quantifies proteinuria) | Helps quantify protein, beyond a dipstick |
| Urine albumin-to-creatinine ratio (UACR) | Albumin loss | Adds detail, especially in milder protein changes |
| Urine microscopy (casts) | What’s in the urine sediment | Can suggest inflammation inside the kidney |
In some centers, clinicians may add an extra blood marker called soluble IL-2 receptor to support the diagnosis when the picture is unclear. It’s not routine everywhere, but it’s one more tool being discussed in recent literature on kidney toxicity from immunotherapy. For a clinician-focused review of diagnosis and treatment, you can see management guidance in Nature Reviews Nephrology.
The red flags to report the same day
Recent clinical guidance puts a lot of weight on how fast creatinine rises. A common “don’t-wait” signal is an increase of about 0.3 mg/dL or 50% above your baseline in serum creatinine, a hallmark of acute kidney injury, especially if it keeps climbing. Also call promptly for reduced urine output, new swelling, or very high blood pressure.
When you call, you can say: “I’m on immunotherapy, and I’m worried about possible nephritis. Can we review my creatinine trend and urine results?”
What usually happens next (so it feels less scary)
First, your team rules out other causes: dehydration, infection, contrast dye, and other kidney-straining meds. Some common culprits include NSAIDs and proton pump inhibitors. Sometimes the fix is fluids and stopping a non-cancer medication.
If interstitial nephritis or acute tubulointerstitial nephritis still looks likely, clinicians often pause immune checkpoint inhibitors like nivolumab, pembrolizumab, or ipilimumab and start steroids for moderate or worse cases, then taper over several weeks if labs improve. Prednisone or other corticosteroids are the standard treatment for acute tubulointerstitial nephritis and interstitial nephritis. For more serious injury from nivolumab or ipilimumab, or if numbers don’t recover, a nephrology consult may follow, and a kidney biopsy, the gold standard for diagnosis, may be discussed to confirm the cause of interstitial nephritis or acute tubulointerstitial nephritis, rule out renal failure, and prevent progression to chronic kidney disease. In severe acute kidney injury, temporary dialysis might be required.
None of this is meant to take hope away. Many people recover kidney function and avoid renal failure or chronic kidney disease with careful monitoring of renal function, and some return to immunotherapy later with careful monitoring. If you’re

