Shortness of breath can feel like it changes the size of the room. One minute you’re talking, the next you’re measuring your words because air feels scarce (dyspnea). If you’ve been told you have a malignant pleural effusion, often seen in lung cancer, you might be wondering what shortness of breath is “normal” for this problem, how to sleep without panicking awake, and when it’s time to stop trying to tough it out at home.
This is one of those cancer side effects that can sneak up, then suddenly demand your full attention. The good news is that there are practical ways to get relief, and there are clear signs that mean you should be seen quickly.
What a malignant pleural effusion does to your breathing (and why it feels worse at night)
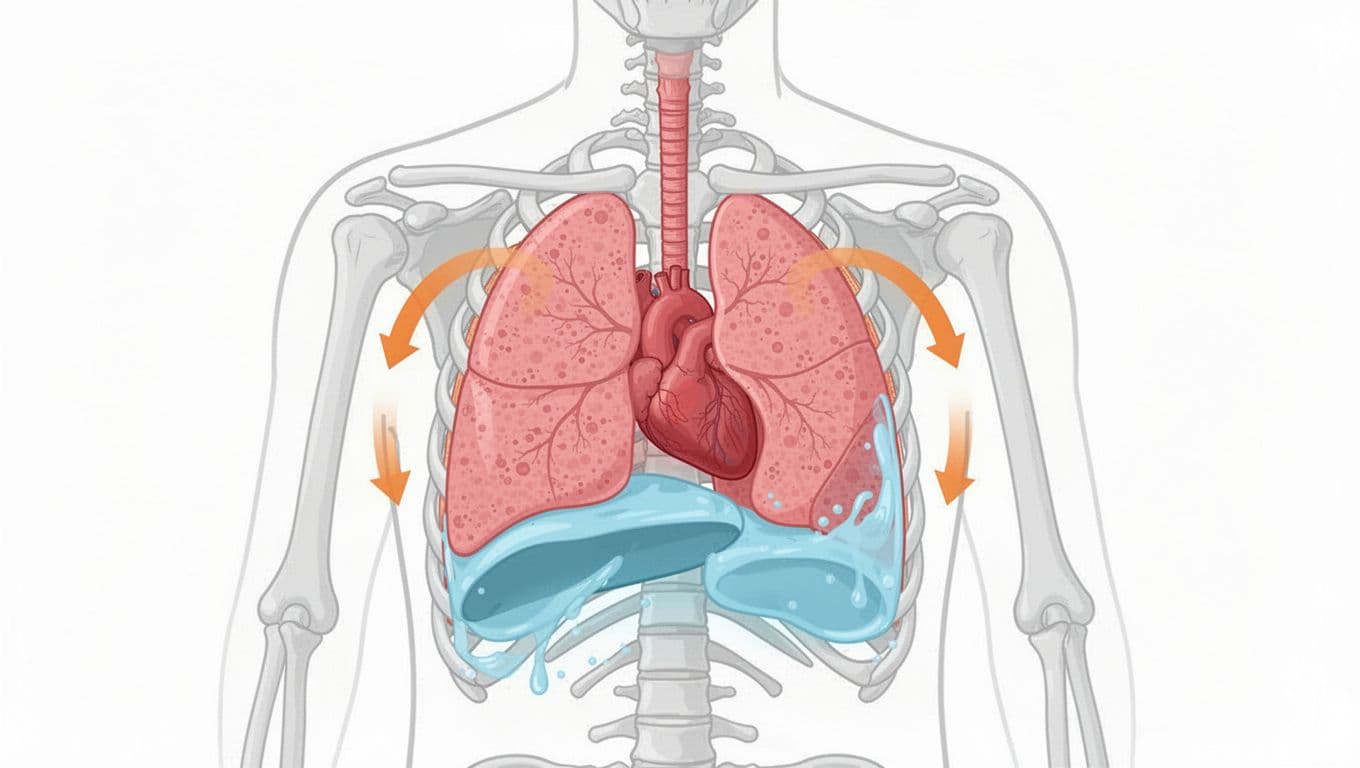
A malignant pleural effusion means fluid buildup in the thin space between the lung and the chest wall (the pleural space) because of cancer. Think of the lung like a soft sponge that wants room to open. This fluid buildup takes up that room, causing lung tissue compression so it can’t expand fully.
The breathlessness pattern often has a few telltale features:
You may notice it builds over days to weeks, not seconds. Walking to the bathroom starts to feel like a small hill. You might need extra pauses when talking. Some people feel a dull heaviness on one side of the chest, or a dry cough that won’t quite quit.
Nights can be harder. Lying flatter lets the fluid spread and shift, and your chest muscles lose the “help” they get from being upright. Anxiety can compound this into nightly panic. If you’ve ever propped yourself up at 2 a.m. and felt relief within a minute, that’s a clue that position matters.
It’s also common for symptoms to come in waves. You may have a “better morning,” then feel shortness of breath tighten up by late afternoon. That swing can be confusing, especially if you’re in treatment or even in remission and trying to trust your body again.
One more important truth: not all breathlessness in metastatic cancer is from pleural effusion. Blood clots, pneumonia, anemia, asthma, and heart strain can copy the same feeling. That’s why clinicians often use imaging and ultrasound to confirm what’s going on, and why treatment choices (draining fluid, placing a catheter, pleurodesis) are tailored to your situation. For a clinician-focused summary of current approaches, see this open-access review from ASCO: Management of Malignant Pleural Effusion in 2024.
Sleeping positions that help when dyspnea prevents a full breath
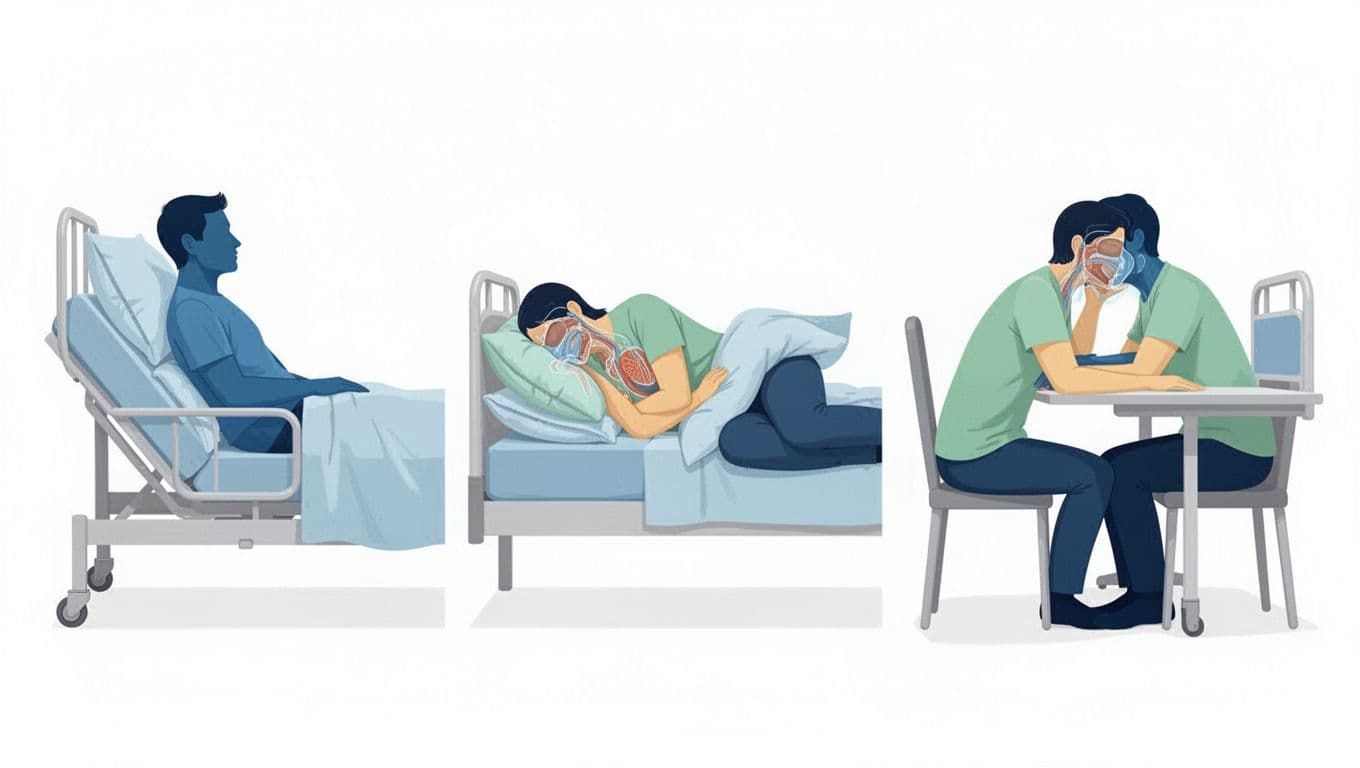
When dyspnea makes breathing hard, sleep can start to feel like a test of courage. Finding the right sleeping positions is key. The goal isn’t perfect sleep. It’s less struggle.
Start with an elevated head. Many people do best in a semi-recumbent position (like a recliner, or in bed with a wedge pillow and a second pillow under the knees). This reduces pressure on the chest and can make each breath feel less “blocked.”
If you prefer side sleeping, use pillows like braces, not decorations, to enhance your sleeping positions. A pillow hugged to the chest can steady the ribs. A pillow behind the back prevents rolling flat. A pillow between the knees keeps the hips from tugging the spine, which can tighten the chest.
Which side should be down? Some people feel better with the affected side down because it splints that side and lets the other side move more freely. Others breathe easier with the healthier side down. Bodies don’t always read the textbook. If you have a home pulse oximeter, let it guide you. If your oxygen drops when you turn, turn back.
When you can’t lie down at all, use the tripod position: sit at the edge of the bed, lean forward slightly, and rest your forearms on your thighs or a pillow on a table. It’s a simple stance, but it recruits breathing muscles that are hard to use when you’re flat.
A few small comforts, often part of palliative care to support quality of life, can stack together:
- Cool air from a handheld fan aimed at your face can reduce the feeling of air hunger.
- Slow breathing out through pursed lips can keep airways open longer.
- Practicing diaphragmatic breathing or other breathing exercises can ease dyspnea.
- Taking meds for pain or cough as prescribed can lower the work of breathing.
For more practical tips on day-to-day breathlessness coping, this patient-friendly guide is useful: managing shortness of breath.
When to call your oncology team, and when to go in right now
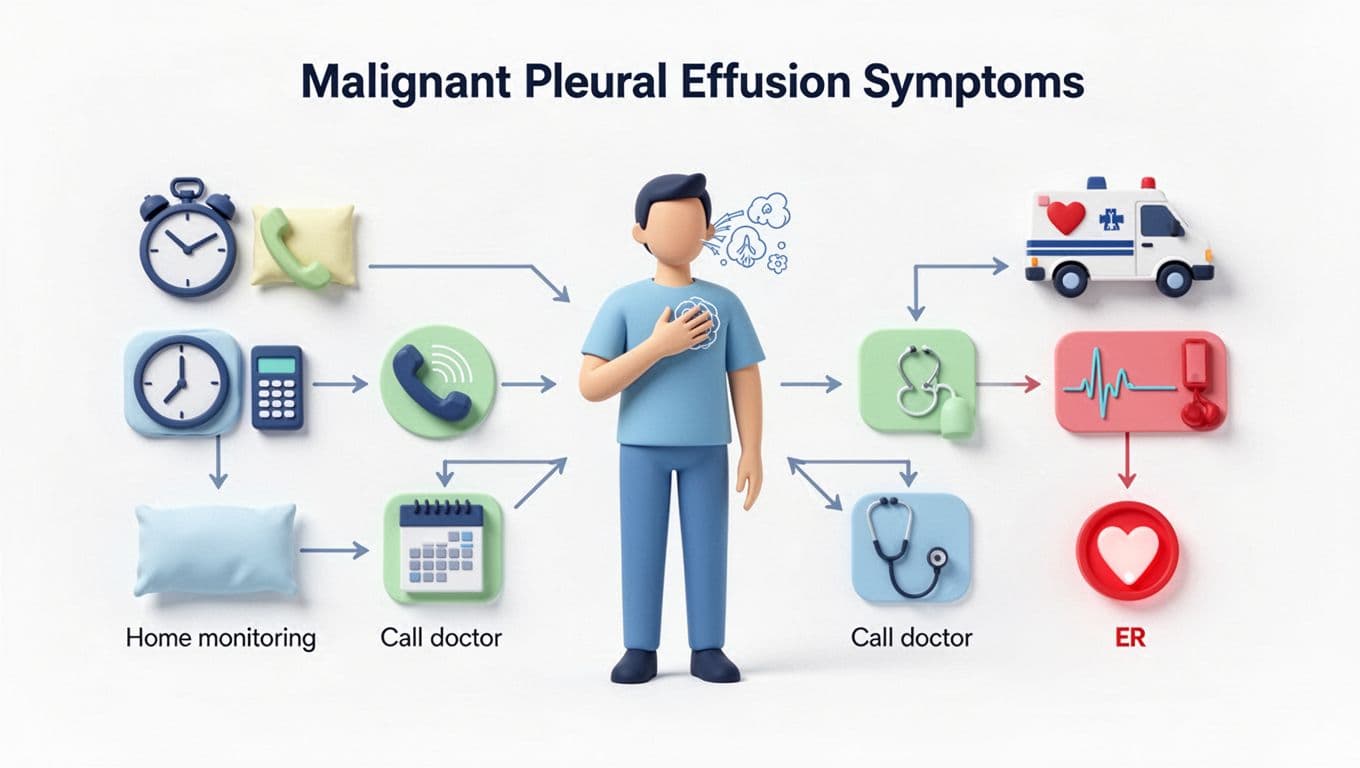
Many people wait too long because they don’t want to “make a fuss.” But breathing trouble isn’t a character test. It’s a body signal.
Here’s a simple way to sort the urgency:
| What’s happening | What to do |
|---|---|
| Mild breathlessness, you can speak full sentences, improves when propped up | Monitor, rest, use your best position, message your team soon |
| Breathlessness is new or clearly worse over 24 to 48 hours, you’re sleeping upright, you can’t do normal tasks | Call your oncology team or on-call line the same day |
| Respiratory distress, blocked airway, chest pain or pressure, fainting, confusion, blue lips, coughing blood, or oxygen very low if you measure it | Go to the ER now or call emergency services |
Also call urgently if you have fever, shaking chills, or new redness and drainage at any chest catheter site. Respiratory infection can move fast.
When you do get evaluated, expect a chest X-ray or ultrasound. Clinicians may offer oxygen therapy as a supplemental tool for those with low saturation, and low-dose morphine or other opioids to manage the sensation of air hunger. If fluid is the main cause, they may recommend thoracentesis (draining fluid with a needle) for quick relief. For fluid that returns, two common longer-term options are an indwelling pleural catheter (a small tube that lets fluid drain over time) or pleurodesis (medicine, often talc, used to help the pleural layers stick together so fluid can’t re-collect as easily). Long-term recovery may involve pulmonary rehabilitation to build breathing strength. A detailed medical overview of these options is summarized here: management of malignant pleural effusions. If you like reading deeper reviews, this 2025 paper also discusses current practice patterns: evidence and best practices review.
If you’re in remission, a new pleural effusion still deserves prompt attention. It may be related to cancer, but it may not. Either way, you shouldn’t carry the worry alone.
Conclusion: breathing support is not “giving in”
A malignant pleural effusion can cause shortness of breath, making breathing feel like work, and it can steal sleep when you need it most. Paying attention to the pattern, using positions that open your chest to reduce anxiety, and knowing your red flags can bring back a sense of control. If symptoms are climbing, ask for help early; palliative care often brings relief. Courage here isn’t pushing through, it’s choosing care when your body asks for it.

