
Immunotherapy can feel like a brave agreement with your future, especially when Cancer has already taken so much. You show up, you take the infusion, you keep going. Then a new kind of tired hits. A headache lingers. Food turns unappealing. You wonder if it’s “just treatment” or something you should name.
One possible cause is immunotherapy hypophysitis, one of the more common immune-related adverse events triggered by immune checkpoint inhibitors that inflames the pituitary gland. It can disrupt hormones that steady your blood pressure, energy, temperature, mood, and more. The good news is that testing is straightforward, and many symptoms improve once hormone replacement begins.
This guide focuses on symptoms you should not brush off and the hormone tests worth requesting.
Why immunotherapy hypophysitis can sneak up on you
The pituitary is small, but it acts like a conductor. When it’s inflamed, the production of adrenocorticotropic hormone (ACTH) and other signaling hormones to other glands can drop fast. This is particularly noted in patients receiving anti-CTLA-4 therapy like ipilimumab. With immune checkpoint inhibitors, your immune system gets better at attacking cancer cells, but sometimes it also attacks healthy tissue.
Hypophysitis from immune checkpoint inhibitors matters because it can cause secondary adrenal insufficiency, meaning your body can’t make enough cortisol. Cortisol helps you handle stress, maintain blood pressure, and keep blood sugar steady. When cortisol falls too low, you can feel awful quickly.
Symptoms also overlap with “normal” treatment fatigue. That overlap is why people often wait. Courage, here, looks quiet. It looks like saying, “This feels different,” even if you worry about being labeled anxious.
For a clinician-focused explanation of recognition and management, see ASCO’s overview on managing hypophysitis. For many patients, the key point is simple: if new symptoms stack up, ask for hormone labs sooner rather than later.
If you’re told it’s “probably dehydration,” it’s still reasonable to ask, “Can we check morning cortisol and ACTH today?”
Immunotherapy hypophysitis symptoms (and the red flags that need urgent care)
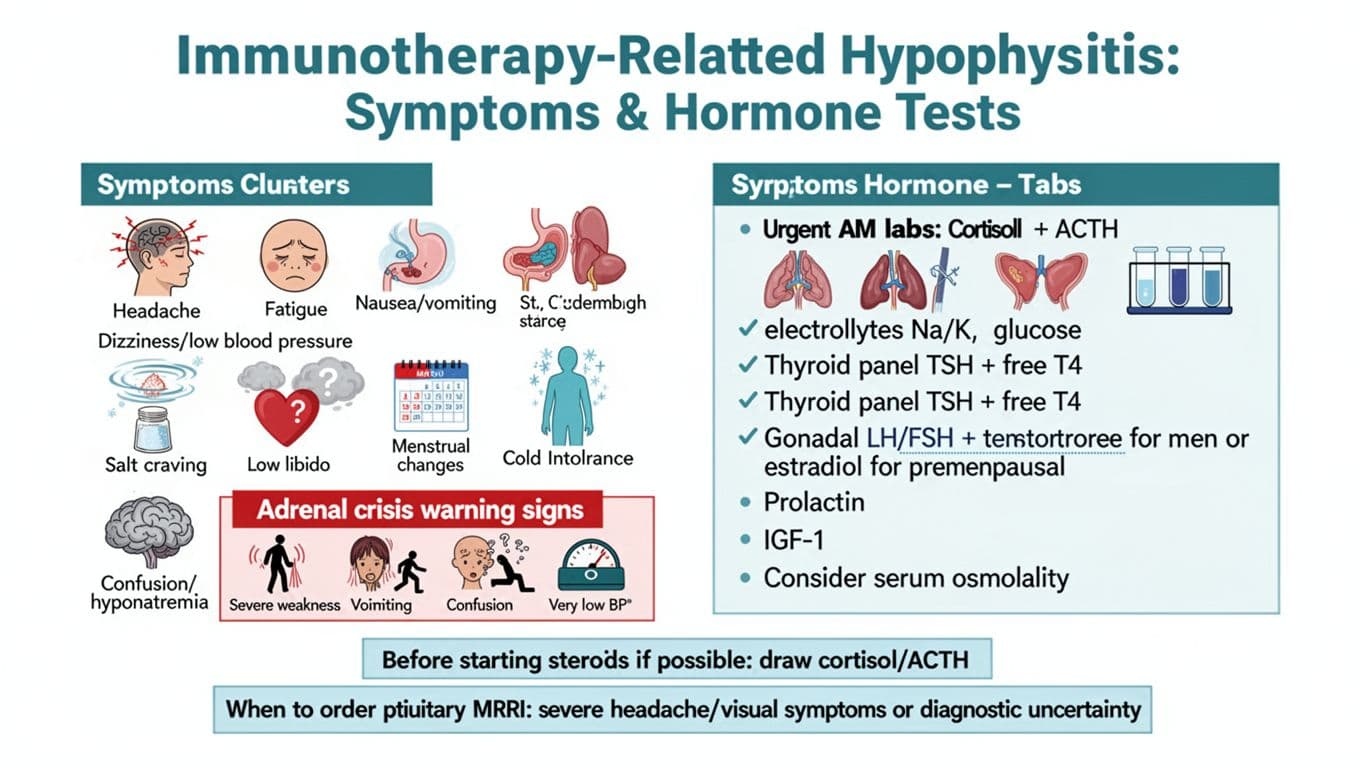
Some symptoms whisper. Others shout. Hypophysitis often starts with a cluster, not a single sign. Pay attention when several of these appear together, especially if they’re new for you:
fatigue and headache are common. So are nausea, poor appetite, and dizziness when standing. Some people notice brain fog, low mood, or feeling unusually cold. Others see changes in sex drive or menstrual cycles.
The most dangerous situation is an adrenal crisis, which can happen when cortisol is critically low, leading to risks like hyponatremia, especially during illness, vomiting, or a bad infection.
Seek urgent care or call your oncology team right away if you have:
- Severe weakness that makes it hard to stand
- Persistent vomiting or you can’t keep fluids down
- Fainting, severe dizziness, or very low blood pressure symptoms
- Confusion or unusual sleepiness
- Severe headache with visual disturbances
If the pituitary is swollen, a condition known as pituitary gland enlargement, it can irritate nearby structures. This is why a magnetic resonance imaging (MRI) scan is often necessary when visual disturbances or severe headaches occur.
For a patient-friendly overview of symptoms, diagnosis, and typical workup, Barrow Neurological Institute’s page on hypophysitis symptoms and diagnosis is a helpful grounding reference.
One more gentle truth: this is not a character test. It’s a body chemistry problem. You didn’t “cause” it by worrying, pushing too hard, or failing to rest.
The hormone tests to ask for (and when timing matters)
When you’re feeling unwell, it’s tempting to accept a quick steroid dose “just in case.” Sometimes steroids are necessary right away. Still, if it’s safe to wait, ask your team to draw morning cortisol levels first, because treatment can blur the diagnostic picture.
Here’s a practical set of labs to discuss for pituitary hormone deficiency. Your clinician will tailor it to your situation, meds, and cancer plan.
| Test | What it helps detect | Why it matters in hypophysitis |
|---|---|---|
| Pituitary hormone deficiency screening | Multiple hormone axis disruptions | Overarching concern when combined labs show drops across pituitary signals and targets |
| 8 AM morning cortisol levels | Low cortisol level | Screens for adrenal insufficiency, often the most urgent issue |
| Adrenocorticotropic hormone | Pituitary signal to the adrenal glands | Helps tell pituitary-related low cortisol from primary adrenal disease |
| Basic metabolic panel (sodium, potassium, etc.) | Low sodium, other electrolyte issues | Low sodium can drive confusion, weakness, and nausea |
| Glucose | Low blood sugar | Low cortisol can drop glucose, adding shakiness and fatigue |
| Thyroid stimulating hormone and free thyroxine | Thyroid hormone status | Screens for central hypothyroidism; in pituitary problems, thyroid stimulating hormone may look “normal” while free thyroxine is low |
| Luteinizing hormone and follicle stimulating hormone | Pituitary signals to ovaries or testes | Explains libido changes, cycle changes, and low sex hormones |
| Testosterone (men) or estradiol (premenopausal) | Sex hormone levels | Helps confirm and guide replacement decisions |
| Prolactin | Pituitary hormone marker | Can shift with pituitary inflammation and supports the overall picture |
| IGF-1 | Growth hormone pathway marker | Not always urgent, but can help assess broader pituitary function |
| Serum osmolality (sometimes) | Hydration and sodium balance context | Useful when sodium is low or symptoms are out of proportion |
A simple way to ask is: “Can we check 8 AM morning cortisol levels and adrenocorticotropic hormone, plus sodium and free thyroxine, today?” That question often gets you to the right first step, especially since ipilimumab often leads to a more comprehensive pituitary hormone deficiency compared to other drugs.
If you want a deeper look at how often hormone axes are affected across studies, this systematic review on hypophysitis frequency and clinical patterns offers useful context.
After the labs: what happens next, and what recovery can look like
If cortisol is low (especially with low or inappropriately normal ACTH), clinicians often start hydrocortisone or other corticosteroids promptly. If thyroid hormone is also low, they usually replace cortisol before starting thyroid hormone, because thyroid replacement alone can worsen adrenal symptoms when cortisol is already low.
Many people also need longer-term thyroid or sex hormone replacement therapy. An endocrinology consult can help with dosing, sick-day rules, and follow-up testing. If headache is severe or vision changes appear, pituitary magnetic resonance imaging (MRI) may be ordered to look for swelling, pituitary stalk thickening, and rule out other causes.
Managing endocrine toxicities like hypophysitis requires a lifelong commitment to hormone replacement therapy for many survivors. Living with hormone replacement therapy can feel like adding another job to an already packed life. Yet many people regain steadier energy and clearer thinking once levels stabilize. Even in remission, it’s worth keeping a short note in your wallet or phone listing adrenal insufficiency and your steroid plan, because emergencies don’t wait for perfect timing.
Conclusion
When your body feels “off” during immunotherapy, you deserve more than guesswork. Immunotherapy hypophysitis is scary mainly because it hides in plain sight, behind fatigue and nausea that seem familiar. While more common with ipilimumab, those on anti-PD-1 therapy like nivolumab or pembrolizumab (especially during combined immunotherapy) should remain vigilant for these immune-related adverse events. Unlike classic lymphocytic hypophysitis, this form is uniquely linked to the specific action of your cancer treatment. Still, the right labs, drawn at the right time, can bring quick clarity. Ask about morning cortisol and ACTH first, then build out the hormone panel with your team. Courage isn’t only enduring treatment, it’s also speaking up early, so you can keep moving toward healing and, with time, remission.

