Face swelling can feel strange and unfair, especially when you’re already carrying the weight of Cancer. One day it’s puffy eyelids in the mirror, the next it’s a tight collar that suddenly won’t close. You might tell yourself it’s “just corticosteroids” or “just fluid,” and sometimes it is.
But sometimes it’s Superior Vena Cava Syndrome (SVCS), a problem that can turn serious quickly. The hard part is that SVCS can start with signs that look almost ordinary, until they don’t.
This guide explains what SVCS is, how face and neck swelling and shortness of breath often show up, simple breathing and positioning tips, and the clear moments when waiting is too risky.
What superior vena cava syndrome is, and why cancer can trigger it
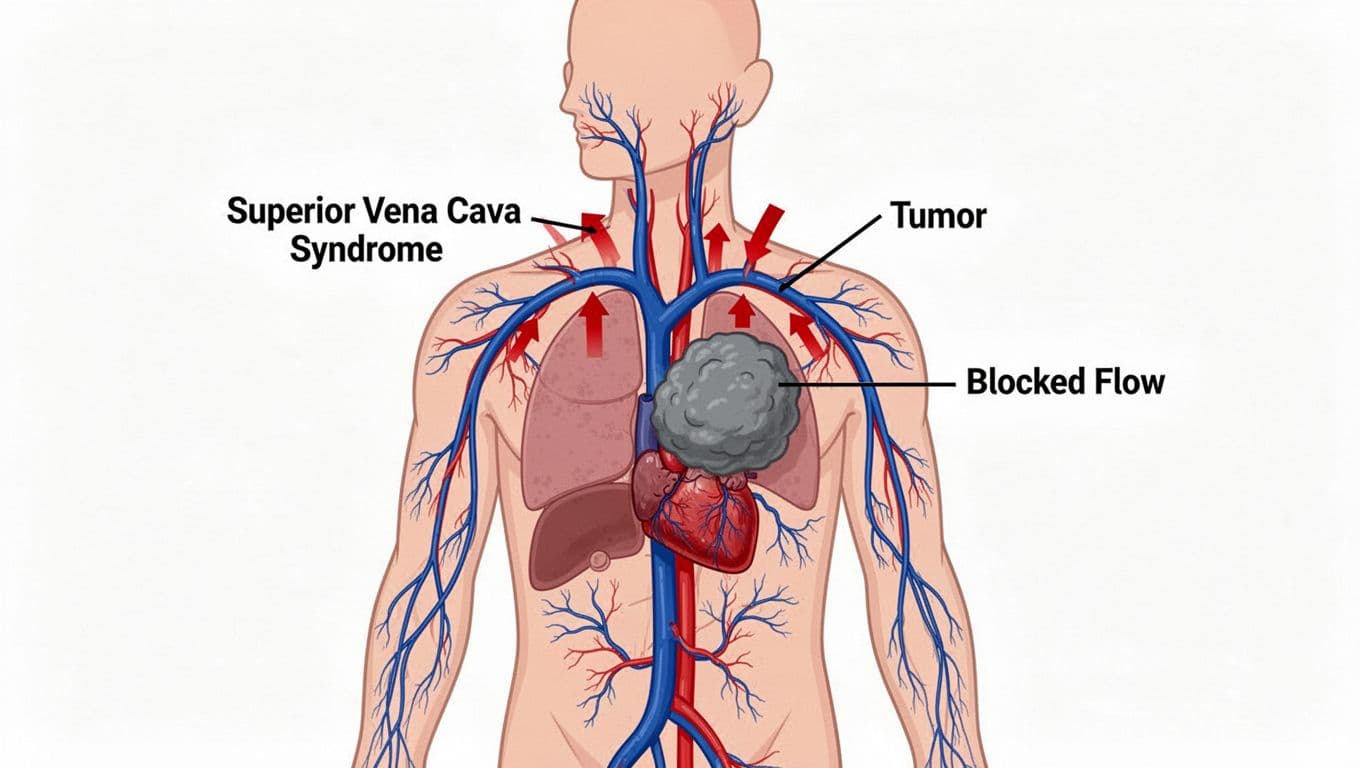
The superior vena cava is a large vein in your chest. Its job is simple: carry blood from your head, neck, arms, and upper chest back to your heart. When that vein gets squeezed from the outside, or blocked from the inside, blood flow is restricted and pressure backs up. Think of it like a busy highway suddenly narrowed to one lane. Traffic piles up, and the “pile up” in your body shows up as swelling and visible veins.
In many adults, Superior Vena Cava Syndrome (SVCS) is linked to cancer in the chest, often lung cancer or non-Hodgkin lymphoma. Research summaries through recent years have found most SVCS cases are caused by malignancy, and in small cell lung cancer it can appear at diagnosis in a noticeable minority of patients. It’s also not only about tumors. Blood clots can do it too, especially if you have a central venous catheter, port, or pacemaker leads.
That’s why SVCS can matter even if you’re in remission. Swelling might come from a clot, scar tissue, or a device related issue, not just tumor growth. Your history changes the odds, but it doesn’t erase the possibility.
If you want a clear, patient-friendly explanation of causes and typical symptoms, the Cleveland Clinic overview of SVCS lays it out in plain language.
Face and neck swelling signs that deserve attention (and the ones that mean 911)
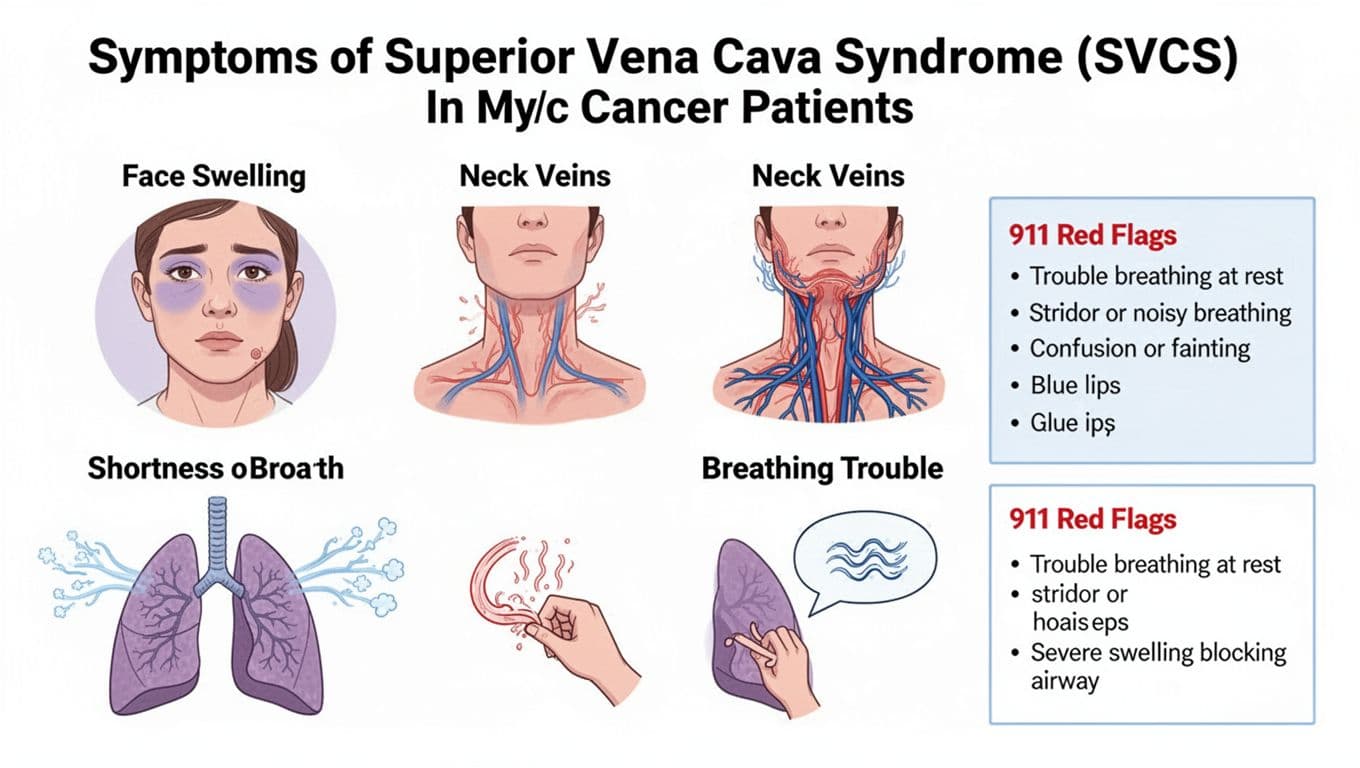
Superior Vena Cava Syndrome (SVCS) often announces itself in the places you can’t ignore: your face, your neck, your breath. Many people notice swelling that’s worse in the morning, or worse when bending forward to tie shoes. Some describe a “full” feeling in the head, like pressure behind the eyes.
Common signs people report include:
- Face puffiness (often around the eyes), or a dusky, reddish face
- Neck swelling or bulging neck veins
- Upper body swelling, swollen arms or hands, rings feeling tight
- Shortness of breath, cough, hoarseness, or difficulty swallowing
- Chest wall veins that stand out more than usual
SVCS becomes a potential medical emergency when swelling and pressure start to affect the airway, breathing, or brain. Don’t try to “tough it out” in these moments. Courage can look like making the call.
Call 911 right now if any of these are true:
- You’re struggling to breathe at rest or can’t speak full sentences
- You have noisy breathing (wheezing or a harsh, high-pitched sound)
- You feel confused, extremely drowsy, or you faint
- Your lips or face look blue or gray (cyanosis)
- Swelling is getting severe fast, especially with throat or tongue symptoms
Rare signs like Horner’s syndrome (drooping eyelid) should also be reported.
SVCS is often described as a 911 emergency and oncologic emergency because it can escalate, and because fast treatment can prevent dangerous complications. OncoLink’s guidance on SVC syndrome as an oncologic emergency can help you see why clinicians take these symptoms seriously.
Breathing tips you can use today, and what treatment may look like
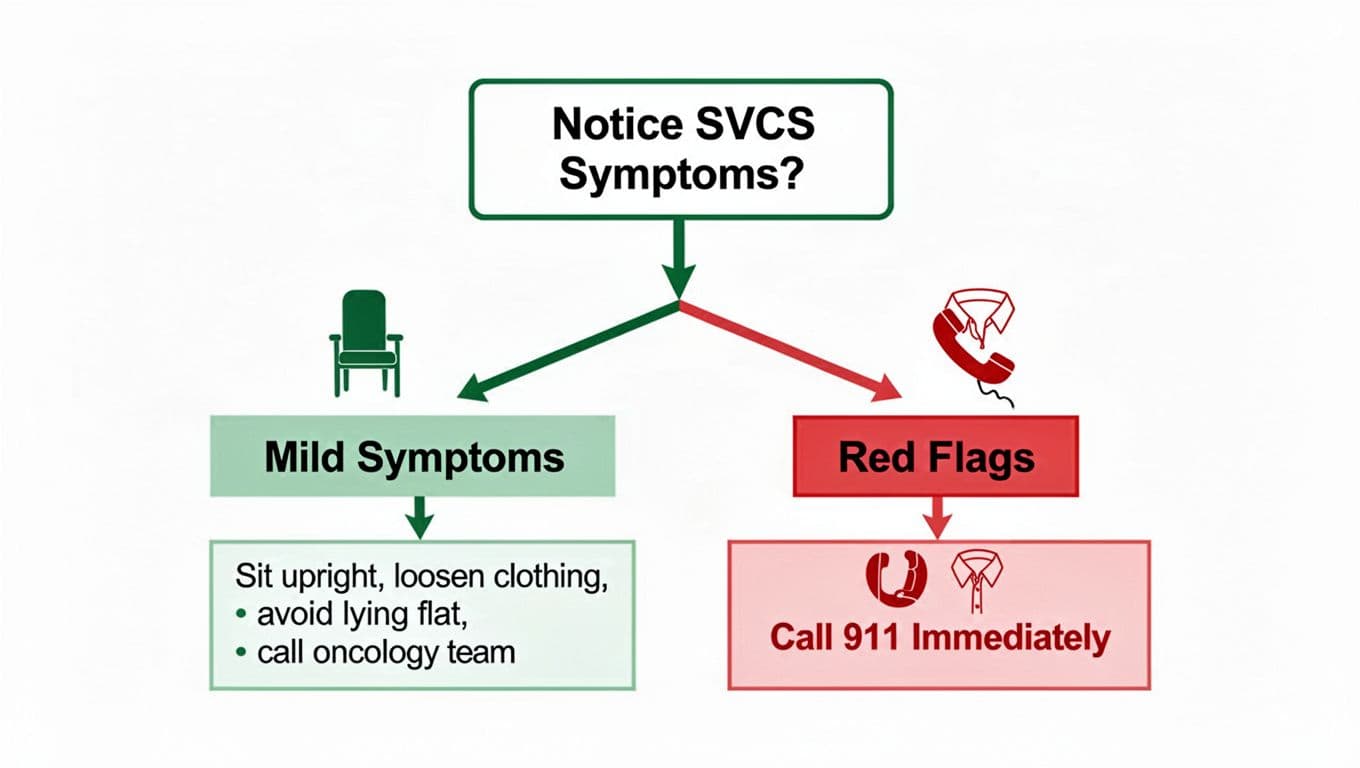
If you suspect SVCS and you’re not in the 911 red-flag zone, your first goal is to reduce pressure and protect your breathing while you contact your oncology team.
Start with small actions that can make breathing easier during trouble breathing:
- Sit upright (or at a strong recline). Avoid lying flat.
- Loosen anything tight around the neck or chest.
- Try “in through the nose, out through pursed lips” for a minute or two.
- Keep talking to a minimum if you’re having trouble breathing, save air for breathing.
- Don’t drive yourself if symptoms are rising quickly or shortness of breath worsens.
This quick table can help you decide your next step:
| What’s happening right now | Best next step |
|---|---|
| New face or neck swelling, mild shortness of breath, stable symptoms | Sit upright, call your oncology team or after-hours line |
| Swelling plus chest discomfort, worsening cough, trouble breathing | Call your oncology team urgently, ask if you should go to the ER |
| Trouble breathing at rest, noisy breathing, confusion, blue lips | Call 911 immediately |
In the hospital, clinicians focus on two tracks: easing the blockage and treating the cause, while monitoring for serious complications like trachea blockage. Diagnostics often start with a chest X-ray, followed by CT scan or venography to map the obstruction. Depending on what’s driving the SVCS, care may include oxygen therapy, diuretics to reduce swelling, thrombolysis or blood thinners if a clot is involved. If symptoms are severe, stent placement inside the vein can bring relief quickly for many people, sometimes within hours to a day. Longer-term treatment often targets the cancer itself with radiation therapy or chemotherapy when appropriate, especially for lung cancer or other tumors causing the compression.
A clinician-facing but readable summary of options, including radiation therapy and chemotherapy, is available in a 2024 review on management of malignant SVCS, and the Canadian Cancer Society page on SVCS explains how it can appear as a cancer-related complication.
Conclusion
Superior Vena Cava Syndrome (SVCS) can feel like your body is waving a flag you didn’t ask for. When that flag is face and neck swelling, a key indicator of this medical emergency, the safest move is to take it seriously and act early. Keep the red flags close, stay upright when symptoms hit, and call for help fast when breathing changes. The brave choice isn’t waiting to see if it passes, it’s protecting your airway and your brain, and letting others step in when you need them most, since prompt action leads to better outcomes. You’re not overreacting, you’re paying attention.

