That small, chronic cough can feel like nothing. A scratch in the throat. A nuisance. After all you’ve carried through cancer, you might be tempted to brush it off and “see if it passes.”
But with Immunotherapy Pneumonitis, a new cough or shortness of breath can be a smoke alarm, not background noise. Immunotherapy Pneumonitis means inflammation in the lungs, and in people on immune checkpoint inhibitors, it can start quietly, then speed up. The brave move isn’t to tough it out. The brave move is early detection and speaking up, especially when noticing these lung cancer symptoms.
This guide is vital for patients with non-small cell lung cancer in treatment and those in remission who still keep one eye on every symptom. You’ll learn what early cough patterns matter, how to use home pulse-ox readings wisely, and when it’s time to stop debating and go to the ER.
The early cough that matters (and why it’s easy to miss)
Immunotherapy drugs (often called checkpoint inhibitors) work by taking the “brakes” off your immune system so it can attack cancer. Sometimes that newly energized immune response irritates healthy tissue too, including lung tissue. That’s immunotherapy pneumonitis, one of the most important “immunotherapy side effects”.
The tricky part is how normal the beginning can feel. Many people describe a dry cough with no mucus, a little more windedness on stairs, or fatigue that doesn’t match the day. It can mimic a cold, allergies, asthma, anxiety, anemia, or simple deconditioning from treatment, and these early signs are often mistaken for common “respiratory infections” or “bronchitis”.
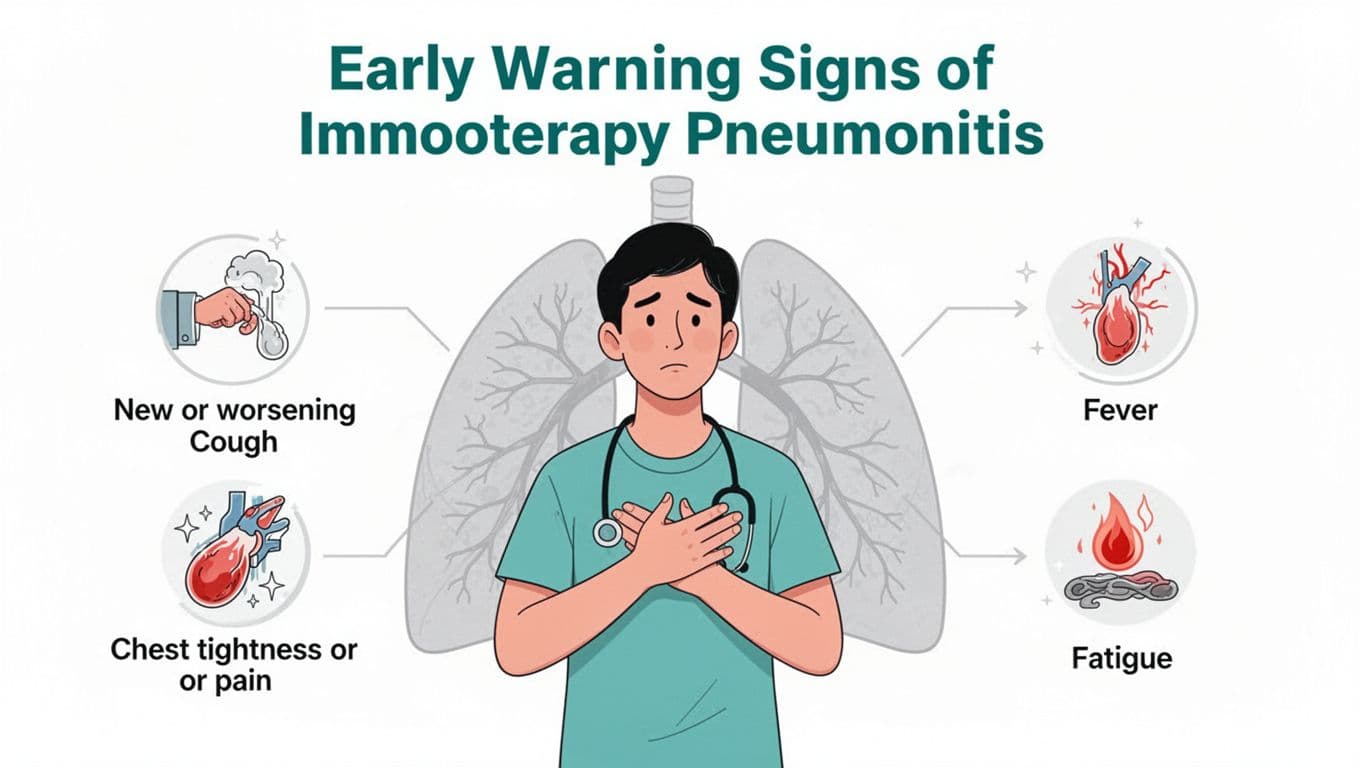
Pay attention to changes that are new for you, especially if they stack up over days:
- A “chronic cough” that’s new, persistent, or clearly worsening
- Shortness of breath doing your usual tasks (showering, walking room to room)
- “Chest discomfort”, tightness, or pain when breathing
- Low-grade fever, chills, or a “coming down with something” feeling
- A sense you can’t get a full breath, even if you’re resting
- New or worsening “fatigue”
- Unexplained “weight loss”
It’s also easy to second-guess symptoms if you’re in remission, such as after treatment for “Stage 1 lung cancer”. You may think, “I’m supposed to be getting my life back, why am I calling again?” Still, immune-related side effects can happen during treatment and sometimes after treatment has paused or ended. Your care team would rather hear from you early than meet you later in crisis.
If you want patient-friendly language about immune side effects (including pneumonitis), the NCCN patient immunotherapy side effects guide is a solid, readable reference.
Home pulse-ox rules that help (without turning you into a hostage to numbers)

A pulse oximeter can be calming or maddening. Used well, it’s a flashlight. Used obsessively, it becomes a strobe light. The goal is simple: catch a meaningful drop in oxygen early, then act.
First, set a baseline when you feel stable. Check your oxygen saturation at rest, sitting up, breathing normally with your pulse oximeter. Write down what’s typical for you. Patients with chronic respiratory conditions like COPD or interstitial lung disease may live at lower numbers, so your clinician’s thresholds matter most.
A few quick technique fixes can prevent false alarms: warm your hands, remove dark nail polish, stay still, and wait for the reading to settle for 30 to 60 seconds.
Here’s a practical guide many oncology teams use for home decisions (your team may set different cutoffs for patients with chronic respiratory conditions):
| Pulse-ox reading (SpO2) | What it can mean | What to do |
|---|---|---|
| 95-100% | Often reassuring | Monitor symptoms, re-check if you feel worse |
| 92-94% | Possible early problem | Call your oncology team today, even if you “feel okay” |
| ≤91% or drop ≥3-4% from your usual | Concerning for low oxygen | Urgent evaluation, often same day, ask where to go |
Two more “numbers” matter as much as SpO2: your trend and your effort. If your oxygen is sliding day by day, or you’re working harder to breathe, don’t wait for a magic low number. Pneumonitis can worsen quickly, and early treatment often means holding immunotherapy and starting anti-inflammatory medicine (often steroids) under medical supervision.
If you want a more clinical deep dive into how immune-related lung toxicity is assessed and treated, the MASCC pulmonary toxicity recommendations outline the medical approach clinicians follow.
When to go to the Emergency Department (and what to say when you get there)
There’s a moment many patients recognize: you start bargaining with yourself. “Let me rest first.” “Let me try one more reading.” “Let me see how I feel after dinner.” Bargaining is human. It’s also dangerous when lungs are involved.
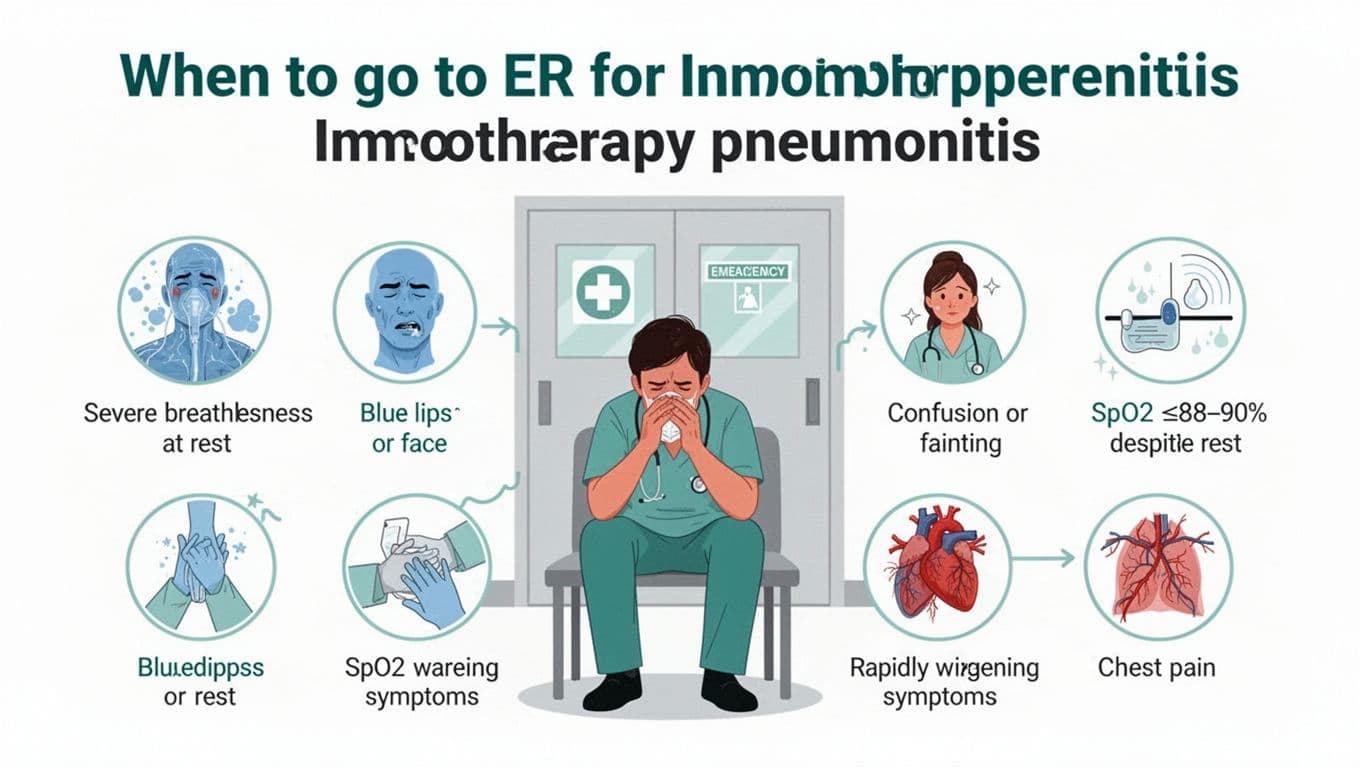
Go to the emergency department now (or call emergency services) if any of these are true:
- You’re shortness of breath or breathing difficulty at rest, or you can’t speak full sentences
- Lips or face look bluish or gray, or someone tells you you look “off”
- You feel confused, faint, unusually sleepy, or you pass out
- Your SpO2 is 88% to 90% or lower (or your team’s red line), especially if it stays low after resting
- Symptoms are rapidly worsening over hours
- You have significant chest pain, especially with breathing
These symptoms often signal the need for immediate hospitalization, particularly persistent breathing difficulty that threatens oxygen levels.
If you arrive at urgent care or the emergency department, say this plainly: “I’m on immunotherapy for cancer, and I’m worried about immunotherapy pneumonitis.” Those words help triage teams think beyond pneumonia, pulmonary embolism, or cardiovascular diseases. You’ll likely be checked for infection and other causes too, because fever and cough can also be flu, COVID, respiratory infections, bacterial pneumonia, coughing up blood, or fluid overload. Imaging tests (often a low-dose CT scan) and oxygen levels help guide next steps, which may require hospitalization.
If you want a trustworthy overview of how clinicians think through diagnosis and treatment, this open-access review on pulmonary toxicity management is thorough without being sensational. For the bigger picture of immune-therapy emergencies, this review of oncologic emergencies from immune-based therapies offers context on why quick action matters.
Conclusion: Courage is calling sooner than you want to
Immunotherapy can be a lifeline, and for many people it supports long stretches of stability or remission. Whether you are receiving immunotherapy, targeted therapy, or radiation therapy, pneumonitis is not a moral failure and it’s not “being dramatic.” It’s a known risk that deserves quick attention.
Trust the early signals: a chronic cough, new breathlessness, and a downward pulse-ox trend. Even those with stage 1 lung cancer should not ignore a chronic cough, as early reporting of symptoms can lead to an improved survival rate. Then choose the courageous thing, call your oncology team, and if red flags appear, go to the ER without waiting. Protecting your lungs is part of protecting your future, and that is worth acting on today.

