Some days, cancer fatigue doesn’t feel like tiredness at all. It feels like gravity got stronger overnight. You might sleep and still wake up worn out, or sit down “for a minute” and realize an hour disappeared.
If you’re in treatment, newly diagnosed, or even in remission, this kind of fatigue can be confusing and lonely. People may see you resting and think you’re getting better. You know the truth: you’re resting because you have to.
Here’s a simple plan you can use on the days your energy won’t cooperate, an “energy ladder” that helps you do what matters, without asking your body for what it can’t give.
Why cancer-related fatigue can feel endless (and when to call for help)

Cancer-related fatigue is common, and it can be stubborn. Recent guideline summaries report that it affects many people during treatment, often 30% to 60%. It can show up from the cancer itself, treatments like chemo or radiation, surgery recovery, pain, poor sleep, stress, low mood, anemia, and side effects from meds. Sometimes it’s one cause. Often it’s a stack of causes, like laundry piled on a chair.
This is also why “just push through” can backfire. When your body is already working overtime, forcing a big burst of effort may cost you for days.
It helps to remember this: fatigue is information, not a moral grade.
That said, some symptoms don’t belong in the “wait it out” box. If you have sudden shortness of breath, chest pain, fever, dizziness or fainting, bleeding, or severe weakness, contact your care team right away. The patient-friendly guidance in the NCCN Guidelines for Patients: Fatigue and Cancer is a solid reference to keep bookmarked, especially when your brain feels foggy.
If your fatigue has changed fast, or it’s new in remission, bring it up. You’re not “complaining.” You’re giving your team data they need.
The Energy Ladder: a simple plan for the hours you can’t spare
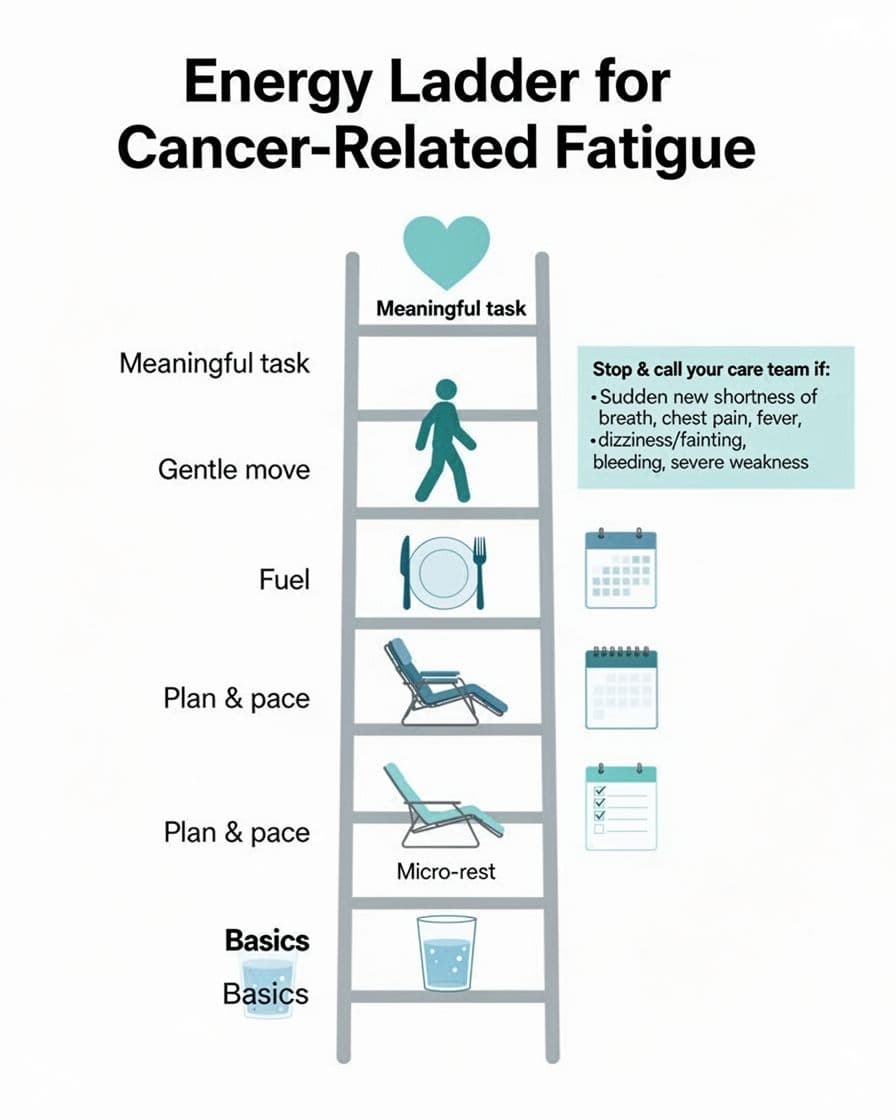
On a hard day, most plans are too big. The Energy Ladder is different. It doesn’t demand a full routine. It offers one rung at a time.
Think of your energy like a small cup, not a bottomless tank. The ladder helps you protect that cup, then decide where to pour it.
How to use the ladder in real time
Start at the bottom. If you can’t do a rung today, stay where you are. You haven’t failed. You’ve listened.
- Basics: Water, meds as prescribed, a cool washcloth, a simple change of clothes. Sometimes the bravest move is meeting the body’s most basic needs.
- Micro-rest: A 5 to 15-minute rest with a timer. Feet up, eyes closed, shoulders dropped. Short rests can refresh you without the “nap hangover.”
- Gentle move: One slow lap inside the house. A few calf raises at the counter. A stretch in bed. Movement can feel unfair when you’re tired, but gentle motion often reduces that heavy, stuck feeling.
- Fuel: Something easy. Yogurt, soup, toast, a smoothie, eggs. Pair carbs with protein when you can, because sugar alone can spike and crash.
- Plan and pace: Pick one task and shrink it. “Laundry” becomes “start the washer.” “Shower” becomes “sit on the edge of the tub and wash hair.”
- Meaningful task: The one thing that makes you feel like you again. A short prayer, a text to someone safe, stepping outside for two minutes, reading one page, folding a child’s shirt. Meaning doesn’t have to be loud to be real.
If you only reach rung two today, that still counts. You are still practicing courage, the quiet kind that doesn’t look impressive from the outside.
Making the ladder work during treatment and in remission

The ladder is simple, but it fits what research keeps finding: small, steady supports tend to beat big, heroic pushes.
For many people, light to moderate exercise helps fatigue over time, even if that sounds backwards at first. The 2024 update from ASCO and the Society for Integrative Oncology highlights exercise, cognitive behavioral therapy (CBT), and mindfulness programs as top options across the cancer journey. If you want to see what that guidance includes, the ASCO guideline update on fatigue in adult survivors is a helpful reference to discuss with your clinician.
Here’s the practical way to blend that guidance with real life:
Choose an “anchor” time. Many people feel best in a narrow window, often late morning or early afternoon. Protect it like an appointment.
Use the two-day rule. If an activity wipes you out for more than 24 to 48 hours, it was too much. Next time, cut it in half.
Practice “energy honesty” with others. A simple line works: “I can do one thing today. Which one matters most?” It turns guilt into teamwork.
If fatigue is tied to worry or low mood, ask about CBT or a structured mindfulness program. That’s not a sign you’re “not coping.” It’s a way to train your brain to stop burning fuel on fear loops.
For a broader clinical view, the ESMO clinical practice guideline on cancer-related fatigue can also give you language for your next appointment.
A closing note for the tired days
Cancer fatigue can shrink a day down to the size of a bedside table. When that happens, the Energy Ladder gives you a next step that fits inside the hour you’re living in.
Try it for a week, not perfectly, just honestly. Track what helps, and tell your care team what you notice. With time, your ladder may change, especially as treatment ends or remission settles in, but the heart of it stays the same: protect your body, pace your effort, and choose one meaningful thing when you can.

