If you’ve ever held a cancer pathology report in your hands, you know the feeling. The paper is quiet, but your mind isn’t. One word can sound like a sentence. One number can feel like a countdown.
A cancer pathology report is not a prophecy. It’s a careful description (such as in a biopsy pathology report) of what the lab can see in the tissue that was removed, measured, stained, and viewed under a microscope. Think of it like a map drawn after a long hike. It doesn’t tell you how strong you are, but it helps you choose the next steps.
This guide walks through the parts people most often ask about, grade, margins, lymph nodes, ER/PR/HER2, and why “positive” can mean very different things depending on the line you’re reading.
Start with the Final Diagnosis: the Cancer Name and Tumor Grade

Most modern cancer pathology reports are easier to scan than they used to be. A cancer pathology report typically includes a gross description (how the tissue looks to the naked eye) and a microscopic description (what is seen under the lens). Many hospitals now use a checklist-style “synoptic summary,” so key facts don’t hide in long paragraphs. When different parts seem to disagree, your care team often treats the synoptic summary as the most reliable snapshot.
Start by finding the Final Diagnosis (or a section with similar wording). This is where you’ll usually see:
- Cancer type (histology): The “what it is” name, such as ductal carcinoma in situ (DCIS), invasive ductal carcinoma, invasive lobular carcinoma, adenocarcinoma, melanoma, lymphoma, and many more. This matters because treatment is built around the type, not just the location.
- In situ vs invasive: “In situ” means the abnormal cells are still contained where they started. “Invasive” means they’ve grown beyond that first boundary into nearby tissue.
- Tumor size: Often in centimeters. Tumor size is one piece used in staging.
- Tumor grade: The “how wild it looks” measure under the microscope.
Tumor grade can feel personal, but it isn’t. It’s about the cells, not you. In plain language, low-grade cells look more like normal cells and tend to grow more slowly. High-grade cells look more abnormal and tend to grow and divide faster. Different cancers use different grading systems, so your report might show Grade 1 to 3, or a named system (like Nottingham histologic grade for breast tissue). The Nottingham histologic grade combines nuclear grade (how abnormal the cell nuclei appear), mitotic rate (how many cells are dividing), and tubule formation.
If you want a friendly walkthrough of common cancer pathology report sections, Breastcancer.org’s pathology report guide lays out the typical headings and what they mean.
Surgical Margins and Lymph Nodes: the lines that show “did we get it all” and “did it spread”
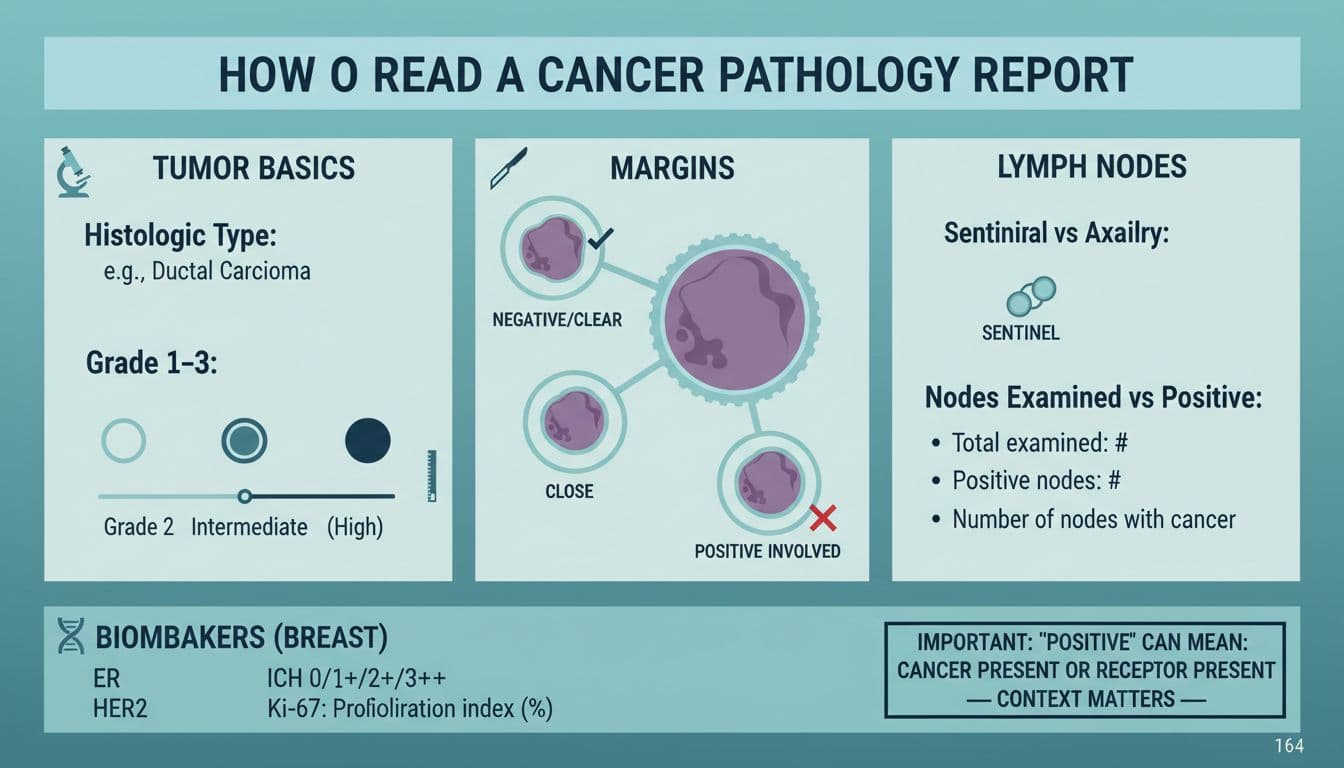
When fear spikes, it often spikes around two words: surgical margins and lymph nodes. Both are trying to answer the same basic question, did any Cancer get left behind, or move beyond the main tumor?
Surgical margins describe the edges of the tissue the surgeon removed. A pathologist inks the outside surface, then checks whether cancer cells touch that ink. Pathologists also examine for lymphovascular invasion near the tumor, which indicates cancer cells have entered nearby lymph or blood vessels and raises concerns about spread to lymph nodes.
- Negative margins usually mean no cancer cells are seen at the cut edge. That’s the goal.
- Positive margins mean cancer cells reach the edge of the specimen, suggesting some may still be in the body at that spot.
- Close surgical margins means cancer cells are near the edge, but not at it. “Close” depends on cancer type and location, so it’s something your surgeon interprets in context.
If the cancer pathology report lists surgical margins by direction (anterior, posterior, medial, lateral), it can feel like reading a compass in a storm. The point is simpler: it tells your team where the closest edge was, so they can decide on re-excision surgery, radiation, or observation.
Lymph nodes are small filters that catch fluid and, sometimes, traveling cancer cells. Cancer pathology reports often list “lymph nodes examined” and “lymph nodes positive.” You might see something like 0/3 lymph nodes or 2/15 lymph nodes.
A few helpful notes:
- The sentinel lymph node is the first node (or first few) most likely to drain the tumor area. If the sentinel lymph node is negative, more extensive lymph node surgery may not be needed, depending on your case.
- A positive lymph node means cancer cells were found in that node, it does not automatically tell you where else cancer is, but it can change staging and treatment.
Surgical margins, lymph nodes, and findings like lymphovascular invasion contribute to the TNM staging system, which helps determine next treatment steps. For more detail on how pathology fits into staging and treatment planning, the American Cancer Society’s explanation of breast pathology reports is a clear, patient-focused reference.
Estrogen Receptor, Progesterone Receptor, HER2 Status, and the Word “Positive”: Same Word, Different Meaning
Estrogen receptor, progesterone receptor, and HER2 status show up most often in breast cancer pathology, and they carry a strange twist: on these lines, “positive” can be good news because it opens doors to targeted treatment.
Here’s the plain-language meaning:
- Estrogen receptor-positive / progesterone receptor-positive: The cancer cells have estrogen receptor or progesterone receptor. Hormones can “feed” these cells, which is why hormone-blocking treatments may help. This hormone receptor status often guides therapy choices.
- HER2 status-positive: The cancer cells make too much HER2 protein (or have extra HER2 gene copies). HER2-targeted drugs can be very effective here.
- HER2 status-negative: HER2 is not overexpressed.
HER2 status is often tested first with immunohistochemistry IHC, reported as 0, 1+, 2+, or 3+. Many labs treat 2+ as equivocal, meaning it’s not clear, and they do a follow-up test (ISH or FISH test) to decide. Your cancer pathology report may list both. HER2 status matters in contexts like ductal carcinoma in situ and invasive ductal carcinoma. Other common tests, such as the Ki-67 test for growth rate, may also appear alongside hormone receptor status in your cancer pathology report.
This is where the word “positive” needs a flashlight, not a panic button. It changes meaning depending on the item being tested:
| Where you see “positive” | What it usually means | Why it matters |
|---|---|---|
| Margin: positive | Cancer at the cut edge | May affect surgery or radiation plans |
| Lymph node: positive | Cancer found in a node | May affect stage and systemic treatment, including for metastatic breast cancer |
| Estrogen receptor/progesterone receptor: positive (hormone receptor status) | Receptors present on cancer cells | Often means hormone therapy is an option; if absent along with HER2 status-negative, it may indicate triple-negative breast cancer |
| HER2 status: positive | HER2 overexpression or gene amplification (confirmed by immunohistochemistry IHC and FISH test if needed) | Often means HER2-targeted therapy is an option |
If you’re in treatment or in remission, these markers including your hormone receptor status and HER2 status can still echo in your follow-up visits. They’re part of your story, but they are not the whole story. The whole story includes how you respond to treatment, your overall health, and the steady courage it takes to keep showing up.
If you want a trustworthy explanation of hormone receptor status (estrogen receptor, progesterone receptor) and HER2 status, Susan G. Komen’s guide to ER/PR and HER2 status breaks it down without talking down to you.
A final practical step: bring your cancer pathology report to appointments and ask your team to translate it out loud. You can use questions like:
- “When the report says positive, positive for what?”
- “Which findings change my treatment plan?”
- “Is anything missing that we still need to test?”
Conclusion: let the report inform you, not define you
A cancer pathology report is a set of facts, measured carefully, written quickly, and read intensely. It provides the final diagnosis to guide the next decision, but it can’t measure your grit, your support system, or your capacity to heal.
As you read each line of the cancer pathology report, keep this close: context is everything, especially with the word “positive.” Take the report one section at a time, write down what you don’t understand, and let your care team carry the medical weight with you. Courage isn’t loud. Sometimes it’s just reading the page, breathing, and asking the next clear question.

