Back pain is common. During cancer treatment, where spinal cord compression in cancer is a risk, it can feel almost expected, a side effect of stress, scans, long days in waiting rooms, or medicines that change how your body feels.
But there’s a type of back pain that doesn’t politely wait for your next appointment. It presses in, night after night, and it asks a hard question: will you act quickly, even if you’re tired of emergencies?
Metastatic spinal cord compression is one of those moments where courage looks plain. It looks like picking up the phone. It looks like saying, “Something’s changed, and I need help now.”
What metastatic spinal cord compression is, and why time matters so much
Metastatic spinal cord compression (often shortened to MSCC) happens when cancer in or near the spine presses on the spinal cord or the bundle of nerves below it (the cauda equina). The pressure can come from a tumor itself, or from a weakened spine bone that collapses. Either way, nerves hate being squeezed.
At first, the only sign might be pain. Then swelling and pressure can start to interrupt nerve signals, causing difficulty walking. Legs may feel heavy. Walking may turn unsteady. Bladder signals may go quiet or chaotic. If compression goes on too long, nerve damage can become permanent.
That’s why clinicians treat MSCC as an oncological emergency. Early treatment can protect the ability to walk and reduce the chance of losing bladder or bowel control. Even if you’re in remission, MSCC still matters because cancer can return or spread silently, and the spine is a common place for metastases.
MSCC is more likely if you have metastasis to the spine (including breast cancer, lung cancer, and prostate cancer), but it can happen with many cancer types. It’s also more likely if you’ve been told you have bone metastases, new spine lesions, or unexplained back pain that’s getting worse.
If you want a patient-friendly list of signs to watch for, the UK acute oncology guidance on MSCC recognition signs and symptoms is clear and practical for spinal cord compression in cancer.
Red Flag Symptoms: The Back Pain Pattern (and the Nerve Symptoms That Often Follow)
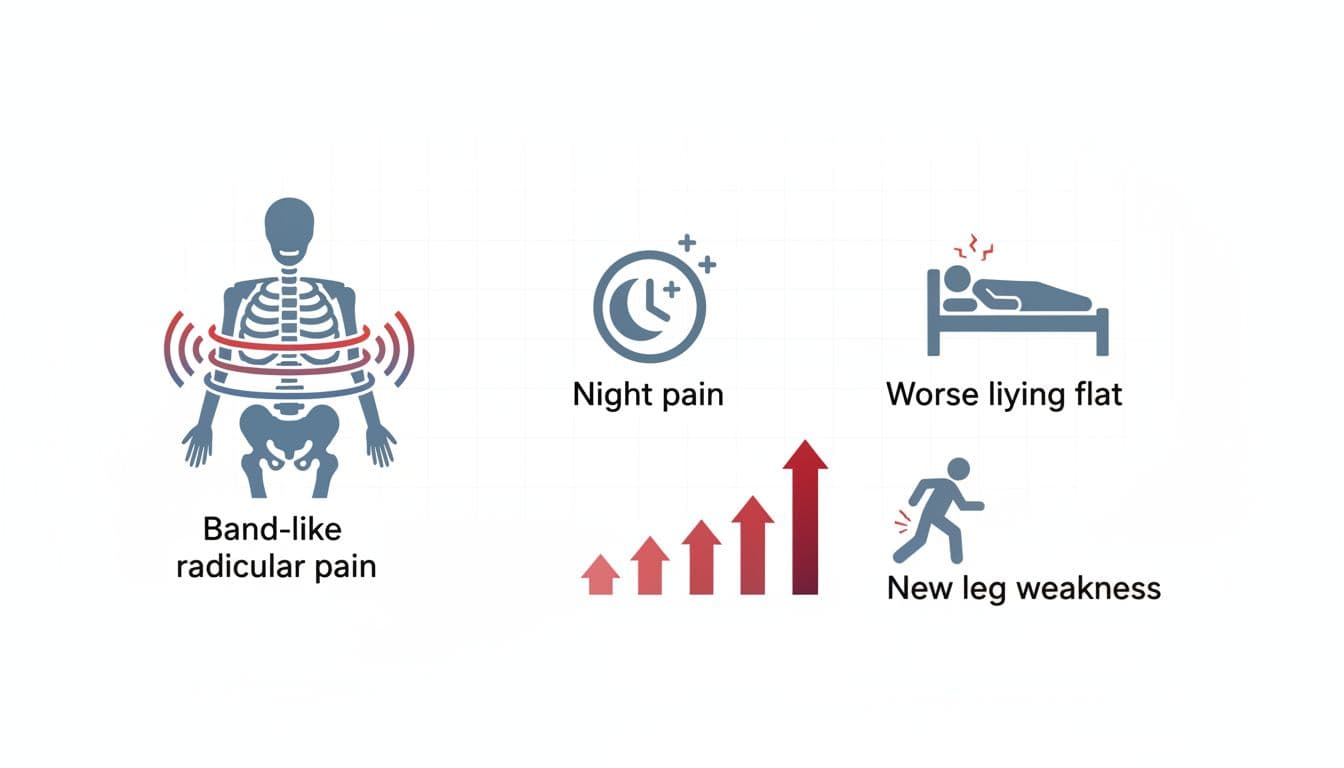
An AI-created infographic showing common red-flag back pain features that can point to spinal cord compression.
“Red flags” can sound dramatic, but the idea is simple: some patterns of pain are more likely to mean “spine and nerves are at risk,” not “I slept wrong.”
With metastatic spinal cord compression, the back pain often has a few recognizable features. It tends to be new or clearly changing, and it usually progresses over days to weeks. Many people notice night pain that wakes them, or pain that feels worse when lying flat. Some describe a band-like pain that wraps around the chest or belly, as if a tight belt is being pulled.
Pain can also shoot down an arm or leg (radicular pain), or sit in the middle of the back (thoracic spine) where “ordinary” strain is less common. Coughing, sneezing, or straining can worsen it.
Then come the symptoms you should never “watch and wait” on, as failing to act on these red flag symptoms can lead to permanent paralysis:
- New limb weakness, heaviness, or trouble standing from a chair
- New sensory loss, numbness or tingling, especially in both legs
- Difficulty walking, unsteadiness, tripping, or falls
- New bladder and bowel dysfunction, especially trouble starting urination or not being able to pee
- Numbness in the “saddle area” (inner thighs, groin)
A helpful way to think about it is this: pain is the smoke, nerve changes are the fire. In metastatic spinal cord compression, early recognition of these signs is critical.
| What you notice | Why it’s a red flag | What to say out loud |
|---|---|---|
| Back pain that’s worsening, night pain, or worse lying flat | Can signal pressure and swelling near the cord | “I have cancer history and new, worsening back pain” |
| Band-like pain around chest or abdomen | Can reflect nerve root irritation | “It wraps around my body like a tight belt” |
| New weakness, numbness, or walking changes | Nerves may be failing under pressure | “My legs feel weaker, and it’s new” |
| Urinary retention or new incontinence | A late warning sign, needs urgent care | “I can’t pee normally, this started today” |
For another perspective on “red flag” nerve symptoms (including bladder and saddle area changes), NICE’s guide to red flag symptoms and signs is a solid reference.
What to do in the first hour: a calm, urgent plan you can follow
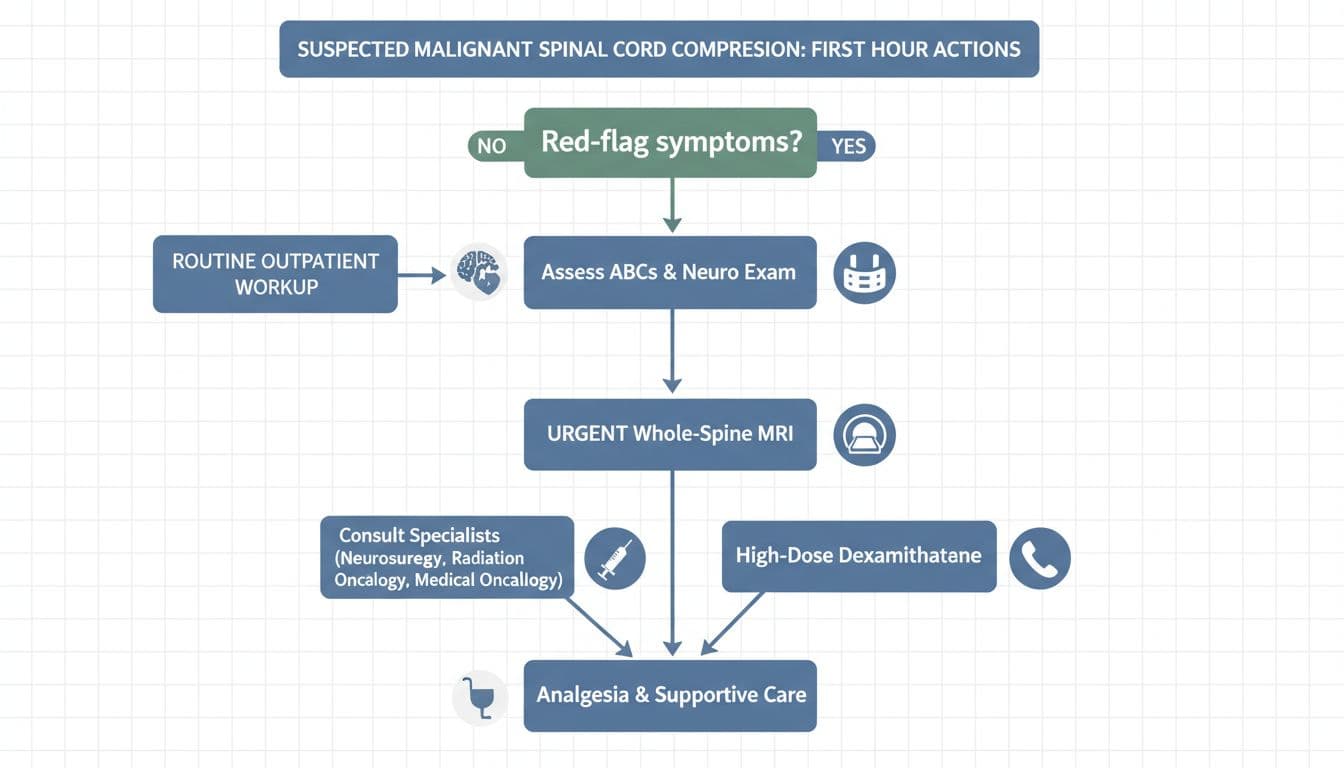
An AI-created flowchart showing the first-hour actions clinicians often take when MSCC is suspected.
When fear hits, the brain likes to bargain: Maybe it’s nothing. Maybe I’ll sleep it off. But the first hour is not about proving you’re “tough.” It’s about protecting your spinal cord with first hour treatment for this oncological emergency.
Here’s a first-hour plan that’s simple enough to use when you’re shaken.
- Call for urgent medical help now. If you have Cancer history plus red-flag back pain, new weakness, numbness, or bladder/bowel changes, treat it as an emergency. If symptoms are severe or progressing, call emergency services rather than driving yourself.
- Say the key phrase clearly: “I’m being treated for cancer (or I’m in remission) and I’m worried about metastatic spinal cord compression.” Those words help the right pathway start faster.
- Limit movement and keep your spine supported. Use bed rest and log-rolling techniques if needed to manage potential spinal instability. Don’t test your strength by walking around “to see if it passes.” If you can, lie flat or stay in a position that keeps your back steady until a clinician tells you otherwise. If moving causes sharp pain or sudden weakness, stop.
- Track and report nerve changes, even if they feel embarrassing. Can you lift each foot? Has numbness spread? When did you last pee, and was it normal? These details guide urgent decisions.
- Gather a fast “handover” list. Cancer type, current treatment, known bone metastases, recent scans, allergies, and blood thinners (anticoagulants). Keep it short and ready.
- Don’t self-start leftover steroids. Clinicians often give dexamethasone quickly to reduce swelling around the cord, but dosing and safety depend on your situation.
What happens on the medical side may include a focused nerve exam for neurological deficit, an urgent MRI scan of the whole spine to identify all lesions, another urgent MRI scan if required, pain control, corticosteroids such as dexamethasone 16mg often given with proton pump inhibitor cover to protect the stomach, bladder care if you can’t urinate, and urgent calls to oncology and spine teams. If you want to understand typical hospital management in plain language, this Management of Spinal Cord Compression summary is a helpful overview of Spinal cord compression in cancer.
After the first hour, treatment for metastatic spinal cord compression may involve radiotherapy, decompressive surgery to relieve pressure and stabilize the spine, or both, with radiotherapy and decompressive surgery often used together. For metastatic spinal cord compression and Spinal cord compression in cancer, radiotherapy plays a key role in many cases, while many people also need rehab. The goal is simple: protect function, reduce pain, and keep your life as intact as possible.
Conclusion
Metastatic spinal cord compression is scary because it moves fast, and because it threatens things we take for granted, like walking to the kitchen or sleeping through the night. Spinal cord compression in cancer shows red-flag patterns, such as back pain and difficulty walking, that signal you to act, not to “wait and see,” especially with histories of breast cancer, lung cancer, or prostate cancer. In the first hour, the bravest move is often the smallest one: call, name the risk, and stay as still as you can until help takes over. If you’re living with cancer, including in remission, you deserve care that treats these warning signs with the seriousness they require.

