Chemo has a way of changing the rules overnight. One week your body feels predictable, the next week it feels like it’s speaking a new language. Constipation during chemo is one of those “nobody warned me it could be this miserable” side effects of chemotherapy, especially when Zofran (ondansetron) for delayed nausea is part of your nausea plan.
Constipation during cancer treatment isn’t just uncomfortable. It can steal sleep, drain appetite, and make you dread the bathroom. The good news is that a calm, step-by-step bowel plan often works, and it can be done safely when you keep your oncology team in the loop.
Why chemo and Zofran can “hit the brakes” on your bowels
Zofran helps many people keep food down, which matters when your body is working hard to heal. The tradeoff is that ondansetron can slow bowel movement, so stool sits longer, dries out, and becomes harder to pass. Add in chemo itself, less activity, less fluid, and sometimes opioid pain meds, and the bowel can start acting like it’s stuck in slow motion.
Here’s what “constipation” can look like in real life:
- Going less often than usual (not just “less than three times a week”).
- Hard stool.
- Straining, rectal pressure, or a feeling of incomplete emptying.
- Abdominal bloating, nausea, stomach cramps, or reduced appetite.
If you want a reliable baseline description of symptoms and common causes, Memorial Sloan Kettering’s patient guide on managing constipation is clear and easy to skim.
The safety piece most people miss
During chemo, “try something and see” can be risky. Suppositories, enemas, and even some supplements can cause problems, especially in the sensitive rectal area, if your white blood cell count is low (infection risk) or platelets are low (bleeding risk). Fiber can backfire if you’re dehydrated or if there’s any concern for narrowing in the bowel.
Call your cancer care team right away if you have:
- Severe or worsening belly pain
- Vomiting
- Fever
- A swollen, hard belly
- No gas passing
- Blood in stool or black stools
This isn’t about being dramatic. It’s about protecting you.
A daily prevention plan (start the same day as chemo)

Think of constipation like a campfire that starts small. If you notice it early, you usually don’t need a rescue mission. Prevention works best when it’s boring and consistent.
1) Fluids with a plan, not a wish
Sip all day, not just at meals. Many cancer centers recommend aiming for generous fluid intake if you’re allowed, and warm non-caffeine fluids can help some people. If you have heart or kidney limits, follow your cancer care team’s guidance.
A simple routine:
- A warm drink in the morning (water, herbal tea, broth, prune juice)
- A bottle or cup you refill on a schedule
- Extra fluids with any added fiber
2) Food choices that don’t fight your gut
During chemo, raw salads and high-fiber foods like whole-grain cereal can feel like sandpaper. Many people do better with soft, cooked foods: oatmeal, soups, stewed fruit, mashed sweet potato, yogurt, scrambled eggs.
Fiber is not always the answer in chemo constipation. If you’re not drinking enough, or if your team has you on a low-fiber plan for any reason, adding fiber can make stools bulk up without moving.
For practical guidance that matches what many oncology clinics teach, the Canadian Cancer Society’s page on constipation during cancer treatment is a steady reference.
3) Gentle movement that tells the bowel to wake up
If walking to the mailbox is all you’ve got today, that counts. Movement helps the gut contract in a more natural rhythm. Short, frequent walks often beat a single long workout.
4) Build a “bowel pattern”
Your bowel likes routines. Many people have more success 5 to 15 minutes after eating or drinking something warm. Use a footstool if it helps you bear down less. Don’t strain like you’re lifting weights.
5) Track it like a symptom, not a personal failing
Write down: last bowel movement, stool hardness, belly pain, nausea, and what you took for relief. This turns guesswork into a clear story your oncology nurse can act on.
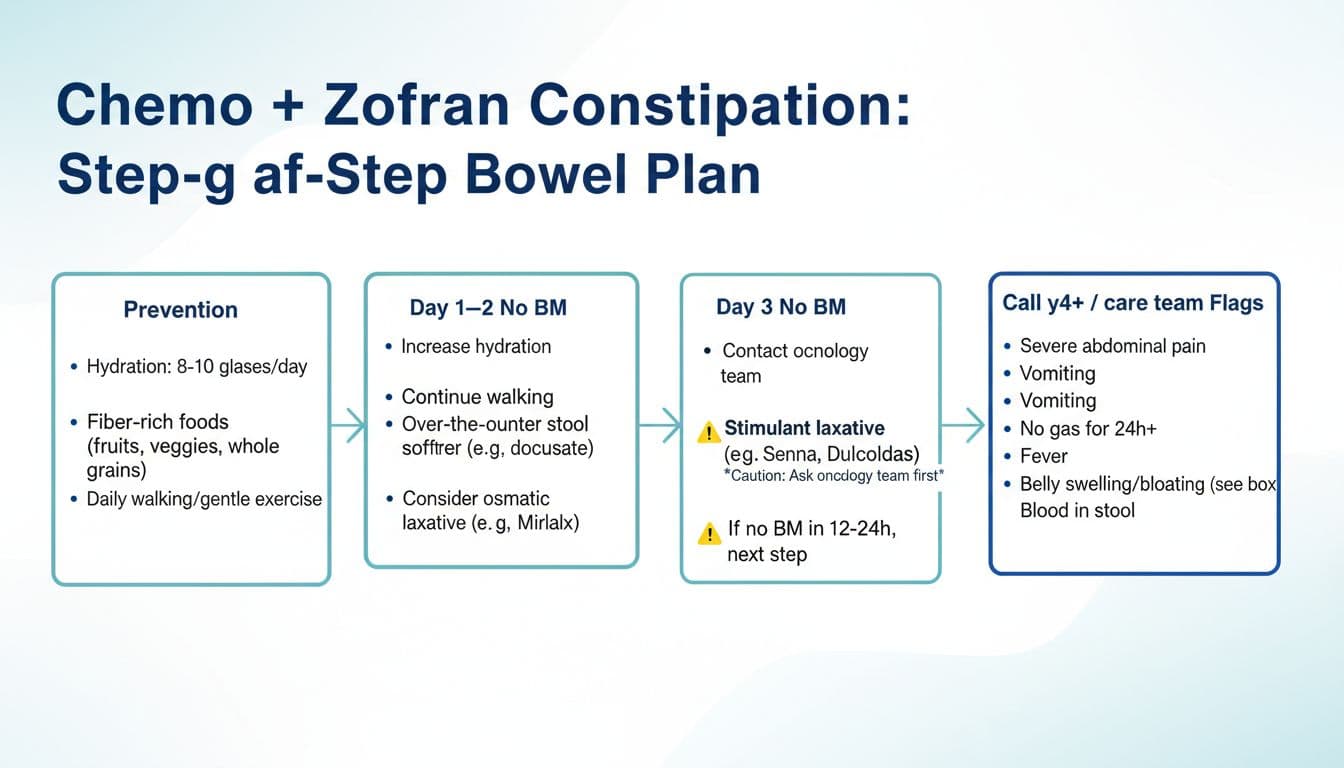
The step-by-step bowel laxative protocol (when you’re already backed up)

This laxative protocol is meant to be safe for many people on chemo, but it still needs your team’s approval, especially if you’ve had bowel surgery, bowel narrowing, severe hemorrhoids, neutropenia, or bleeding risk.
A simple escalation table you can follow
| Timing | What to do | What to avoid |
|---|---|---|
| Prevention (daily) | Fluids, warm drink in the morning, short walks, cooked foods, bathroom routine, track symptoms | Sudden high-fiber foods without fluids or approval |
| Day 1 to 2 with no bowel movement | Keep fluids up, walk if you can, ask your team if a stool softener is appropriate for hard stool, consider an osmotic laxative plan if they approve | “Wait it out” if you’re getting more bloated or nauseated |
| Day 3 with no bowel movement | Call your oncology team for next-step guidance, they may suggest an osmotic plus a stimulant laxative depending on your meds and exam | Suppositories or enemas unless your team says it’s safe |
| Day 4+ or red flags anytime | Call urgently, you may need same-day evaluation to rule out impaction or blockage | Any home “force it” approach |
What the common options actually do (in plain language)
Stool softeners help stool hold onto moisture. They can be helpful when stool is dry, but they may not be strong enough alone when Zofran is slowing movement.
Osmotic laxatives pull water into the bowel so stool can move more easily. Options like PEG (such as Miralax) or Milk of Magnesia, and lactulose syrup, are common; many teams use these early because they’re less “crampy” for some people.
Stimulant laxatives trigger bowel contractions. They can be the right tool, especially when the gut has slowed from meds; sennosides like Senokot-S are examples, but your team may want you to use them in a planned way.
Suppositories and enemas can be effective for some situations, but during chemo they come with extra caution. A Dulcolax suppository is one option, though if your counts are low, the risk-benefit changes.
For a clear, medication-focused handout style overview, BC Cancer’s guidance on constipation caused by medications explains why your medication list matters so much.
If you’re on opioids, don’t wait
Opioids and Zofran together can turn constipation into a fast-moving problem. If you take opioid pain medications, ask for a bowel routine the same day you start it. This is one of those small acts of courage that pays off quickly.
Conclusion: small steps, steady relief, and a safer road forward
Chemo asks for courage in ways nobody trains for, including the quiet courage of paying attention to your body’s signals. Constipation during chemo, one of the common side effects of chemotherapy, can feel embarrassing, but it’s a medical side effect, not a character flaw.
Start prevention early, escalate by days (not by frustration), and call your cancer care team when the clock is ticking or symptoms change. Managing these issues can help with anticipatory nausea by reducing overall physical distress. Whether you’re newly diagnosed, in active treatment, or in remission, bowel health is part of comfort, strength, and healing.

